- ECG criteria for sinus bradycardia
- Causes
- Nursing interventions
- Treatment
Sinus Bradycardia ECG/EKG Nursing Review
 Sinus: means it’s a type of sinus rhythm (this rhythm is originating from the SA node)
Brady: slow cardia: the heart’s action
Bradycardia: slow heart action
Normal heart rate: 60-100 bpm
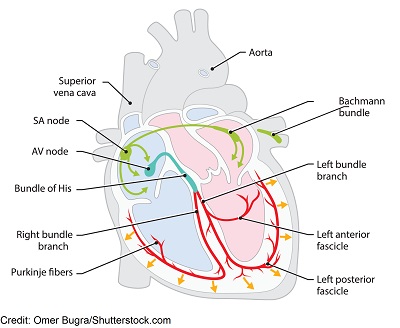
The SA node, which is the sinoatrial node, is known as the pacemaker of the heart. If it’s working like it should, the heart should beat at 60-100 bpm. But in some cases the SA node is firing at a slower rate, and this produces a heart rhythm known as sinus bradycardia.
Therefore, sinus bradycardia is a heart rhythm that meets the criteria for normal sinus rhythm (originating from the SA node), but has a slow rate of less than 60 bpm.
Sinus: means it’s a type of sinus rhythm (this rhythm is originating from the SA node)
Brady: slow cardia: the heart’s action
Bradycardia: slow heart action
Normal heart rate: 60-100 bpm
The SA node, which is the sinoatrial node, is known as the pacemaker of the heart. If it’s working like it should, the heart should beat at 60-100 bpm. But in some cases the SA node is firing at a slower rate, and this produces a heart rhythm known as sinus bradycardia.
Therefore, sinus bradycardia is a heart rhythm that meets the criteria for normal sinus rhythm (originating from the SA node), but has a slow rate of less than 60 bpm.
ECG/EKG Study Guide and Workbook for Nursing Students
“ECG/EKG Interpretation Study Guide and Workbook by Nurse Sarah”. This book contain 100 pages of content featuring 26 ECG rhythm break downs, 51 ECG rhythm analysis practice problems, 100 comprehensive ECG practice questions, worksheets, chart summaries, and more.
You can get an eBook version here: “Nurse Sarah ECG Book” or a physical copy here: “ECG/EKG Interpretation Study Guide by Nurse Sarah“.
Criteria for Sinus Bradycardia:
How can you know if your patient is presenting with sinus bradycardia? Make sure the heart rhythm meets the criteria for normal sinus rhythm and it has a rate of less than 60 bpm. To help you do this, ask yourself the following questions (covered in the ECG interpretation basic video): PQRST: P wave: 3’s R’s (regularity of rhythm, rate, resemblance)- P wave: regularity of rhythm is present in the p waves, rate of less than 60, resemblance: only one p wave in front of each QRS complex, round and upright (uniform throughout)
- QRS complex: regularity of the rhythm is present in the QRS complexes, rate less than 60, QRS present with each p wave, measures less than 0.12 seconds
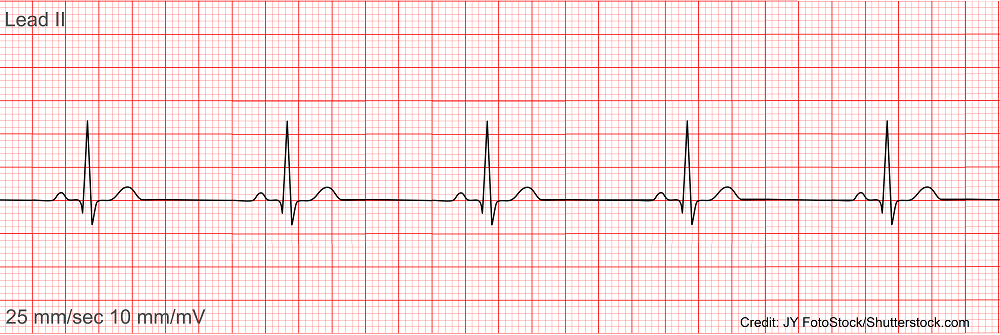 P waves: regular, atrial rate of 50 bpm, one p wave is present with each QRS, upright and round, measures 0.10 seconds
QRS complexes: regular, ventricular rate of 50 bpm, present after each p wave, measures 0.12 seconds
T wave: present
Extras: PR interval 0.20 seconds, ST segment flat, QT interval: 0.36 seconds
Interpretation: sinus bradycardia with a rate of 50 bpm
A finding of sinus bradycardia doesn’t always mean something is wrong with your patient and they need medical treatment immediately, but in some cases it does require immediate attention.
To know if it is a bad sign for your patient: You have to assess if your patient is having signs and symptoms from the slow heart rate (Symptomatic Bradycardia: fainting, fatigues easily, confused, chest pain, dizzy, difficulty breathing, low blood pressure etc.) and what the cause could be.
P waves: regular, atrial rate of 50 bpm, one p wave is present with each QRS, upright and round, measures 0.10 seconds
QRS complexes: regular, ventricular rate of 50 bpm, present after each p wave, measures 0.12 seconds
T wave: present
Extras: PR interval 0.20 seconds, ST segment flat, QT interval: 0.36 seconds
Interpretation: sinus bradycardia with a rate of 50 bpm
A finding of sinus bradycardia doesn’t always mean something is wrong with your patient and they need medical treatment immediately, but in some cases it does require immediate attention.
To know if it is a bad sign for your patient: You have to assess if your patient is having signs and symptoms from the slow heart rate (Symptomatic Bradycardia: fainting, fatigues easily, confused, chest pain, dizzy, difficulty breathing, low blood pressure etc.) and what the cause could be.
Causes of Sinus Bradycardia
“Slow Rates” Sick Sinus Syndrome (the SA node is damaged severely so it can’t work as the pacemaker of the heart) and this condition can lead to other dysrhythmias sinus arrest or brady-tachy syndrome Low thyroid hormone Older adult (as some humans age so does the SA node and this causes the heart to beat slower) Weak & damaged heart muscle (ischemia “myocardial infraction” damage to the SA node from decreased blood supply, inflammation/infection “pericarditis“) Raised Intracranial pressure: part of Cushing’s Triad (slow heart rate, irregular respirations, and widened pulse pressure) Athlete (well-conditioned) Toxicity of: beta blockers “olol”, calcium channel blockers “verapamil”, clonidine, digoxin Electrolyte imbalances (hyperkalemia.. severe cases) Stimulation of vagal response: overactive or vomitingSinus Bradycardia Nursing Interventions & Treatments
Nursing: if patient is symptomatic and becoming unstable activate the emergency response system in your facility, place on oxygen is having dyspnea, confirm IV access, place on bedside cardiac monitor and monitor vitals (heart rate, blood pressure, respiratory rate), assess lung and heart sounds (crackles or extra heart sounds, which could demonstrate congestive heart failure), hold any medications that slow the heart rate down, protect from injury (risk of falling), have lifesaving medications and equipment close by Treatment: Find and treat the cause: medication: stop it, electrolyte imbalance: fix it etc. Medications: Atropine (rapid IV push: 1 mg every 3-5 mins…no more than 3 mg per ACLS guidelines)- doesn’t work if patient has a transplanted heart
- blocks the effects of the vagus nerve (this nerve connects to the SA Node and causes it to slow down the rate) so this medication will help increase the heart rate
- If not effective a drip of dopamine (increases heart rate and blood pressure), or epinephrine may be used
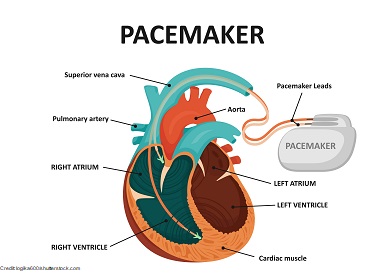 Pacemaker:
Temporary (transcutaneous pacing): may be used when patient not responding to medications like atropine and epinephrine and is unstable
Pacemaker:
Temporary (transcutaneous pacing): may be used when patient not responding to medications like atropine and epinephrine and is unstable
- pacing pads are applied to the skin and electrical discharges are sent through skin to the heart muscle to cause depolarization of the heart so it contracts and beats at a normal rate
American Heart Association. (2020). Adult Bradycardia Algorithm – American Heart Association CPR [Ebook] (p. 1). Retrieved 4 March 2022, from https://cpr.heart.org/-/media/CPR-Files/CPR-Guidelines-Files/Algorithms/AlgorithmACLS_Bradycardia_200612.pdf.
How the Heart Works | NHLBI, NIH. Retrieved 15 February 2022, from https://www.nhlbi.nih.gov/health-topics/how-heart-works
Sattar Y, Chhabra L. Electrocardiogram. [Updated 2021 Jul 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK549803/
