What are some things that nurses should know about their patients in order to provide great care? How can nurses remember all of the many tasks required during each shift? In this article, I’ll tell you some common things nurses should know, as well as tips for how to keep it all organized.
Things Nurses Should Know
When you work as a nurse, things can get extremely busy. Not only do you have to deal with patients with a variety of health issues, but you also have to remember to plan for tasks that you’ll have to do during your shift, such as changing IVs, administering medications, and so forth.
Below is a list of some common things that nurses need to know, as well as some tips on how to find this information and remember it throughout your shift.
Keep in mind that this list is a general guide, not an exhaustive list. You may need to know more (or less), depending on your specialty and patient population.
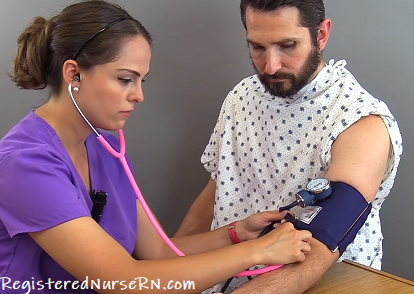
Know the Patient’s Diagnosis and Health History
You’ll want to know why your patient is in your healthcare facility in the first place. Why are they receiving treatment?
In addition, you’ll want to know the patient’s health history, as this will help you determine specific things to watch for during your shift. For example, if your patient has diabetes, you’ll want to watch out for hypoglycemia or hyperglycemia, check their blood sugar as needed, watch their diet, and so forth.
Know the Patient’s Allergies
Knowing your patient’s allergies is also important. You don’t want accidentally to cause harm or discomfort to your patient by giving them a substance to which they are allergic.
Furthermore, if you don’t know the patient’s allergies, you might get a doctors order for a medication that they patient can’t have, and then have to go to the trouble of calling the doctor back to get a new medication. That’s never fun.
Know the Patient’s Code Status
Next, you’ll want to know how to respond if your patient codes. Is your patient a full code or a DNR (do not resuscitate)? If they are a full code, it means that the healthcare team will intervene in a code situation. In a do not resuscitate (DRN), no intervention will take place. You can also discuss code status with your patient to ensure they know what will happen.
This is important to know because there may be a situation in which the patient seems to improve and is even in the process of being discharged, yet they can suddenly code.
Know the Patient’s Lab and Testing Results
By knowing the patient’s lab and testing results, you’ll be able to know pertinent information that will allow you to make necessary clinical decisions to keep your patient in good health.
For example, you’ll want to look at trending labs. If you’re monitoring hematocrit and hemoglobin, is it going up or down?
You’ll also want to know about any pending labs or procedures the patient may need so that you can collect labs on time and prepare the patient for any procedures (example: keep patient from eating if they are NPO – nothing by mouth).
Know the Patient’s Diet Status
Another important thing to know as the nurse is the patient’s diet status. Can the patient eat? If so, can the patient feed himself or herself?
Some patients will be required to follow a specific diet. For example, your patient may be on a cardiac diet, renal diet, or a soft diet, which is often ordered when the patient has difficulty swallowing.
Know Your Patient’s Baseline Health Status
Knowing your patient’s baseline health status is also very important. You’ll want to know things like your patient’s vital signs and mental status.
What kind of heart rhythm has the patient been running? Are they running sinus rhythm, sinus tach, atrial fib, or atrial flutter?
It’s also good to know the patient’s abilities. Isi the patient a total care patient, or can they perform tasks such as walking themselves to the bathroom.
Know the Patient’s Venous Access
You’ll want to determine whether the patient have venous access, and if so, where it is located. What size gauge was used, and when does it need to be changed per your facility’s protocols?
Know the Patient’s Medications
You’ll want to know what medications the patient is on and the time you’ll need to administer them. Some medications are time-sensitive or require lab work prior to administration, so it’s important to know that information.
Pain medications are often prescribed “as needed,” so you’ll want to know when the patient can have more if they request it.
Fluids are also important to know, and these can be as simple as saline solutions, but you may also have drips that you have to titrate based on the patient’s vital signs or lab results.
Know Your Patient’s Devices
Your patient may have internal or external devices that you’ll need to consider or assess. For example, your patients may have devices such as a pacemakers, sub-q ports, wound vacs, drains, or feeding tubes.
Know the Patient’s Physician Groups
In many cases, physician groups will be consulted for patients with certain health problems. You’ll want to be familiar with those physician groups so that you can contact them if your patient requires further care.
Know the Patient’s Plan of Care
As a nurse, you’ll want to be familiar with the patient’s plan of care. You can often find this information in the physician’s progress notes.
If you take time to read what physicians have been documenting about the patient, it can help give you a better understanding of how to care for your patient.
Know the Patient’s Support System
Your patient may have designated family or friends to know about their health status, and it’s important to know this information so that you can keep the patient’s loved ones informed.
How to Find Your Patient’s Information
Now that you know some things that nurses should know about their patients, let me tell you how you can find this information.
You’ll learn most of this information during report hand-off, which you will receive from the nurse you relieve. You can also assess the patient yourself and ask any questions to know everything you need to know to provide great care.
If you failed to get any information during nursing report or from the patient, you can also access important information from the patient’s chart.
How to Remember Your Patient’s Information and Stay on Task
That’s how you find the information you need to know, but how are you supposed to remember all of those details, especially when you have multiple patients with different health problems?
What I have found helpful is to use a nursing report sheet template. You can print and use the free template on our website or create your own to fit your specialty or patient population.
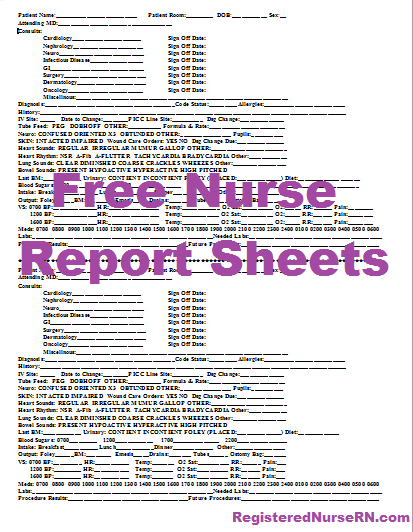
By using a report sheet template, you can quickly fill in details about patients during report, and check it as often as needed to keep up with medication administration, when to change IVs, and all of the other tasks and information that I mentioned previously. They can be very helpful in guiding you through your shift and helping you keep things organized.
However, just keep in mind that you’ll want to follow HIPAA and your facility’s protocols to keep your patients’ health information secure and private, including what patient identifying information you include on any templates and the method you use to dispose of it.