This abnormal rhythm originates from the electrical components in the AV junction, primarily the AV node or potentially the bundle of His, as a result of increased automaticity. This indicates that the cells in the AV node are more energized than usual, leading to accelerated function, resulting in the heart beating consistently without external stimulation.
When this occurs, it overrides the heart’s primary pacemaker (the SA node). In instances of accelerated junctional rhythm, the SA node may be generating electrical signals at a slower rate (resulting in decreased automaticity), leading to the AV node assuming control.
Check out the lecture on accelerated junctional rhythm below and don’t forget to take the free review quiz on accelerated junctional when you’re done reviewing this material.
How will this rhythm manifest? Let’s start by discussing how a typical ECG waveform is generated by the electrical conduction system, then we can contrast that with what is observed in accelerated junctional rhythm.
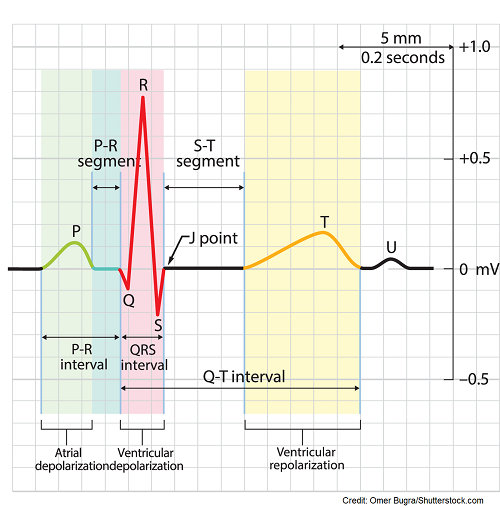
The electrical signal typically originates in the SA node situated in the upper section of the right atrium, acting as the primary pacemaker of the heart and regulating a heartbeat of 60-100 bpm. When activated, it transmits electrical signals downwards across the atria, triggering depolarization in the cells of both the right and left atrium, resulting in their contraction. Consequently, this produces a distinctive upright and easily visible P wave preceding each QRS complex.
ECG/EKG Study Guide and Workbook for Nursing Students
“ECG/EKG Interpretation Study Guide and Workbook by Nurse Sarah”. This book contain 100 pages of content featuring 26 ECG rhythm break downs, 51 ECG rhythm analysis practice problems, 100 comprehensive ECG practice questions, worksheets, chart summaries, and more.
You can get an eBook version here: “Nurse Sarah ECG Book” or a physical copy here: “ECG/EKG Interpretation Study Guide by Nurse Sarah“.
Then, the electrical signals proceed to the:
- AV node (atrioventricular node): located in the lower part of the right atrium just above the tricuspid valve, this node acts as the heart’s “gatekeeper.” It serves as a backup pacemaker and can take control if the SA node is sluggish or malfunctioning, regulating the heart rate to 40-60 bpm.
- The AV node is recognized for introducing a delay in electrical signaling to allow the atria time to empty blood into the ventricles. Without this delay, incomplete blood emptying from the atria to the ventricles could lead to complications.
- Then it’s time for the ventricles to be depolarized (hence contract). The electrical signal travels down to the bundle of His (the third type of pacemaker beating around 20-40 bpm).
- Next, the signal branches off into the bundle branches (right and left).
- Finally, the signal reaches the Purkinje fibers, leading to ventricular depolarization. This creates the QRS complex.
- Following this, repolarization takes place creating the T wave, and the cycle repeats continuously.
Result if everything is firing as it should:
Normal ecg waveform with one upright P wave in front of one QRS complex, normal PR interval 0.12-0.20 second, normal QRS complex <0.12 second, normal QT interval and T waves.
In accelerated junctional rhythm, the electrical components in the AV junction (which can be the AV node or Bundle of His) experience an elevation in their action potential. Typically beating at around 40-60 bpm, in this rhythm, their automaticity increases, leading them to assume the role of the heart’s primary pacemaker. The electrical impulses will proceed through the ventricles as usual, resulting in a regular rate with a normal but narrow QRS complex (<0.12 seconds), a normal QT interval and T wave.
However, the electrical signal travels upwards through the atria (instead of downwards), causing a retrograde effect that alters the appearance of the P waves on the ECG.
Key Characteristics to remember:
- Rate 60-100 bpm and regular
- QRS narrow <0.12 seconds, normal QT interval and T wave
- P waves abnormal and appear upside down (inverted) in leads II, III, aVf
- The p wave can be found in any of these places:
- concealed (hiding in the QRS complex)
- behind the QRS complex…no PR interval in this case
- before the QRS but be very close to it leading to a short PR interval <0.12 seconds
- The p wave can be found in any of these places:
Jingle to remember:
Inverted P on aVF, 2, and 3,
Before or after QRS, if you can see.
Sometimes it hides, and you can’t see it at all,
but when it appears in the front, the PR interval is small.
Causes of Accelerated Junctional Rhythm
- main cause is from digoxin toxicity
- damage to the heart muscle: myocardial infarction (inferior infarct)
- inflammation of the heart “myocarditis”
- after heart surgery
Nursing’s Role and Treatment for Accelerated Junctional Rhythm:
Assess for symptoms: Are they having symptoms?
No: Keep monitoring without requiring treatment. Often, patients do not exhibit symptoms, because they are able to maintain cardiac output with a heart between 60-100 bpm.
Symptoms may occur when electrical signals prompt the ventricles to contract before the atria, disrupting the atria’s ability to empty into the ventricles due to retrograde signals. This alteration affects the volume of blood, resulting in decreased cardiac output.
Keep an eye out for signs of low cardiac output, such as shortness of breath, low blood pressure, dizziness, chest pain, increased capillary refill time, and a weak pulse.
Assessing for Causes:
- The primary cause is digoxin toxicity, which can be treated with the antidote DigiFab.
- Check the level of digoxin, which should be between 0.5 to 2 ng/mL (levels above 2 ng/mL are toxic).
- Monitor electrolyte levels, particularly potassium (high or low levels), calcium, magnesium, and sodium, as they influence muscle contraction.
- If symptoms of decreased cardiac output present, temporary pacing may be required.
References:
Hafeez Y, Grossman SA. Junctional Rhythm. [Updated 2023 Feb 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507715/
How the Heart Works | NHLBI, NIH. Retrieved 15 February 2022, from https://www.nhlbi.nih.gov/health-topics/how-heart-works
Thaler, M. S. (2010). Arrhythmias of Sinus Origin. In The Only EKG Book You’ll Ever Need (6th ed., pp. 110–111). essay, Lippincott, Williams, Wilkins.