Fluid volume deficit occurs because there isn’t enough fluid in the body to support bodily needs and functions. This is sometime referred to as hypovolemia or dehydration.
Dehydration can occur due to a loss of water or certain electrolytes like sodium, not taking in enough water or sodium, or something happens to cause the water in the body to shift around in the fluid compartments. For example, when water moves from the intravascular to interstitial compartment through a process called third-spacing.
In this review, you will learn about the types of fluid volume deficit, signs and symptoms, treatments, and nursing interventions.
Don’t forget to take the fluid volume deficit quiz and to watch the lecture on hypovolemia.
Nurse Sarah’s Notes and Merch
Just released is “Fluid and Electrolytes Notes, Mnemonics, and Quizzes by Nurse Sarah“. These notes contain 84 pages of Nurse Sarah’s illustrated, fun notes with mnemonics, worksheets, and 130 test questions with rationales.
You can get an eBook version here or a physical copy of the book here.
Fluid volume deficit affects the fluid compartments of the body by depleting them of fluid.
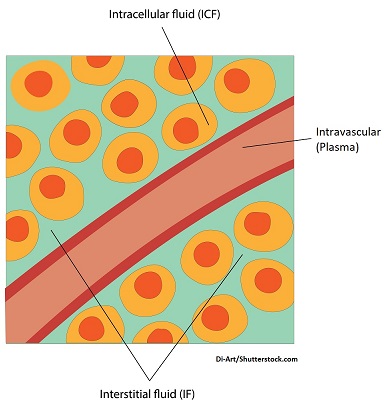
Let’s quickly review these compartments:
Remember there is the intracellular compartment which is the fluid found inside the cell, and it accounts for 2/3 of our body water.
The extracellular compartment is the fluid outside the cell and accounts for 1/3 of our body water.
This compartment can be further divided into:
Intersitital space: the fluid surrounding the outside or in between cells
Intravascular space (this the blood plasma): the fluid found within our blood vessels
Transcellular space: this is the fluid found around joints and certain organs (it is the smallest extracellular compartment of the three).
These compartments can become depleted of fluid and depending on the cause or type of deficit the patient has will determine which compartment is the most affected.
Types of Dehydration
Hypertonic dehydration: occurs mainly due to a loss of WATER rather than electrolytes (hence solutes…sodium). This type can also be called hypernatremia (high sodium in the blood).
When we’re talking about the term hypertonic, we’re talking about things that cause the extracellular compartment to become very concentrated with solutes especially sodium (it will have less fluid).
- Hypertonic means the extracellular fluid has a high osmolarity and is highly concentrated of solutes, particularly of sodium.
- Results: in these conditions water is going to move from the intracellular compartment to the extracellular compartment and the cell is going to shrink and become dehydrated.
- Treatment for this would be to rehydrate the cell by administering hypotonic fluids.
Causes: think of causes that make the blood concentrated
- Losing water: severe cases of diarrhea/vomiting, diabetes insipidus: passing high volumes of urine due to low ADH (antidiuretic levels)
- Not taking in enough water: impaired thirst
Hypotonic dehydration: occurs mainly due to a loss of ELECTROLYES (solutes which is sodium) rather than water. This type can also be called hyponatremia (low sodium in the blood).
- Hypotonic means the extracellular fluid has a low osmolarity and a low concentration of solutes, particularly sodium.
- Results: in these conditions water is going to move to the extracellular compartment to intracellular compartment and the cell is going to swell. This will deplete the extracellular compartment.
Causes: think of causes that lead the body to lose electrolytes (particularly sodium) or dilutes solutes
- Too much diuretics like thiazides (waste too much sodium)
- Too much hypotonic solutions…loss of solute concentration because this fluid dilutes it
- Starvation or malnourishment (not consuming enough electrolytes)
Isotonic dehydration: occurs because there is an equal loss of water and electrolytes
- no drastic shifting of water between compartments
- most common type seen
- problems arise from intravascular loss (losing fluid to pump through out the body) and can lead to hypovolemic shock
Causes:
- Diuretics
- Third-spacing (water shifts from intravascular space to interstitial)
- Bleeding out
- Vomiting/diarrhea/sweating
Signs and Symptoms of Fluid Volume Deficit
“Dehydrated”
Dry mucous membranes
Early sign: increased heart rate (pulse will feel weak)
Hypotension: not a lot of blood volume to pump and occurs as postural hypotension (orthostatic hypotension)
- This is a form of hypotension that occurs when the patient goes from a supine or sitting position to a standing position. This can happen up to 3-5 minutes after the position change.
- Make sure you have a baseline blood pressure and then measure the patient’s blood pressure in these different positions (sitting, standing, supine).
- To have this: “the patient’s systolic blood pressure decreases at least 20 mm Hg or diastolic blood pressure decreases at least 10 mm Hg.”- Bradley, J. G., & Davis, K. A., 2003
Young babies: sunken fontanelles
Decreased skin turgor (skin elasticity): not applicable to geriatric patients because as a patient ages skin elasticity decreases naturally
Refill to capillaries sluggish (greater than 3 seconds)
Attitude changes: restless, confused, lethargic, and progress to seizures (mental status changes means severe case of dehydration)
Thirsty (not all patients will have this): in geriatric patients the thirst response decreases and young patients may not be able to communicate they are thirsty
Experience weight loss: 1 kg (2.2 lbs) = 1 Liter of fluid…patient weights are a good indicator of fluid status
Diagnostics: lab results are going to depend on the type of dehydration (for example hypotonic dehydration may present with different lab values), but most commonly there is a low amount of fluid so blood and urine is going to be concentrated. Therefore, the tests that check for blood and urine concentrations will be INCREASED.
- Increased serum osmolality (blood)
- Increased hbg and hct
- Increased BUN
- Increased Na+ level (not the case of hypotonic dehydration)
- Increased urine specific gravity and osmolality (NOT the case with patients who have diabetes insipidus because urine will be diluted from low levels of ADH)
Nursing Interventions for Dehydration
Goal is to replace the water and electrolyte deficit.
Find the cause and treat it! We play a role with:
- Weighing the patient DAILY (same time, same scale): assess if the patient is gaining or losing weight. Remember a patient’s weight is a great early indicator of patient’s fluid status
- Strict intake and output tracking: know exactly what patient is taking in (IV fluids, flushes, oral and tube feedings, irrigation) and putting out (urine, vomit, suction etc.)
- Monitor urine output closely to make sure kidneys are functioning and if hydration status is improving: want urinary output for the adult to be a minimum of 30 mL/hr or 0.5 mL/kg/hr
- Treatment with oral hydration (make sure patient has easy access to healthy hydration sources…avoid teas and coffee type drinks)
- Administering IV fluids per doctor’s order:
- IV fluids used depends on the cause. Typically, isotonic fluids, but if cause is hypertonic dehydration (hypotonic fluids may be used), and if hypotonic dehydration (hypertonic may be used)
- Monitor electrolyte level (sodium)
Test your knowledge with this dehydration quiz.
References:
Bradley, J. G., & Davis, K. A. (2003, December 15). Orthostatic hypotension. American Family Physician. Retrieved April 28, 2023, from https://www.aafp.org/pubs/afp/issues/2003/1215/p2393.html)
Lopez MJ, Hall CA. Physiology, Osmosis. [Updated 2023 Mar 13]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557609/
Taylor K, Jones EB. Adult Dehydration. [Updated 2022 Oct 3]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK555956/
U.S. National Library of Medicine. (2021, November 6). Fluid imbalance: Medlineplus medical encyclopedia. MedlinePlus. https://medlineplus.gov/ency/article/001187.htm