A cataract nursing review for students prepping for the NCLEX exam!
Cataracts are a type of eye disorder that can cause blindness. This review will cover the following:
- What are Cataracts?
- Pathophysiology of Cataracts
- Signs and Symptoms of Cataracts
- Causes of Cataracts
- Treatment
- Nursing Interventions for Cataracts
Don’t forget about the free cataracts NCLEX questions quiz after the review.
Cataracts Nursing Review
What are cataracts? It’s an eye disorder that occurs when the lens of the eye loses its transparency. As a result, the transmission of light to the retina is affected, which leads to vision impairment. This impairment is described as cloudy, murky visual perception.
This is an example of the type of vision experienced by someone with cataracts:

Cataracts are a common eye disorder, especially in older adults. In fact, according to the National Eye Institute:
“more than half of all Americans age 80 or older either have cataracts or have had surgery to get rid of cataract.” -National Eye Institute
Pathophysiology of Cataracts
How do our eyes actually see images and how does the lens of the eye play a role in this?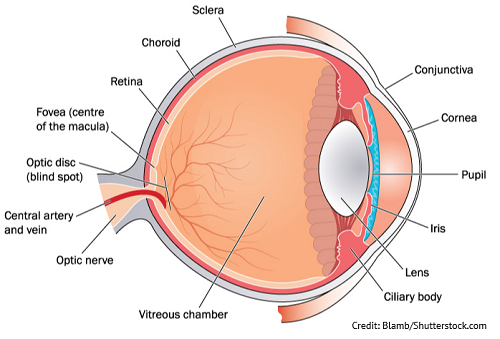
There are many structures in the eye that work together to allow us to see and process images. It all starts with light. When we open our eyes light is detected and enters through the cornea, which is the outer most part of the eye. If you look at the side of someone’s eye, many times you can see this small clear outward bulge that envelops the middle of the eye. The cornea helps process the light received through the eye by bending it so it can get to its proper destination.
Now, under the cornea is the iris (the colored part of the eye and there are various shades of eye colors which make us unique). Within the middle of the iris, is the pupil (which is simply a hole). The iris is made up of smooth muscle that will contract and relax depending on the amount of light detected by the eye. The goal of the iris is to be a gatekeeper so just the right amount of light enters the eye, and it does this by increasing or decreasing the diameter of the pupil.
For example, if a lot of light is detected by the eye, the iris will cause the pupil to constrict and this helps prevent too much light from entering the eye. Then, on the flip side, if more light is needed to process images, the pupil will cause the pupil to dilate. This is an automatic feature we can’t control.
Once the light passes through the pupil it hits the lens. The lens has special muscles attached to it called ciliary muscles. These muscles will help bend the lens so you can focus on objects depending on their distance. Therefore, these muscles are responsible for accommodation.
Also, the lens should be transparent (very clear) due to being made up of clear proteins called crystallin. Crystallin gives the eye lens its clarity and helps the light focus onto the retina.
The retina has very special receptors that are sensitive to light called photoreceptors (specifically cones and rods). These neat receptors turn the light received by the eye into electrical signals and transmits them through the optic nerve and into the brain. Once there we are able to see the most vibrant, clearest image possible.
What happens in conditions like cataracts?
In most cases of cataracts (due to the aging process that causes senile cataracts) the lens starts to become cloudy. This is because crystalline proteins start to stick together and this clouds the lens.
Think of it like a dirty window….when a window is dirty; the light coming in through the window scatters and visual perception of the room is poor. However, if the light comes in through a clean window, the light beams through the room creating excellent visual perception.
Therefore, with a cloudy non-transparent lens, the light breaks up or scatters which causes the light not to reach the photoreceptors properly. This causes the images to be visualized as cloudy and blurry at any distance. Eventually, as the lens continues to become more cloudy the retina will receive less light and the lens can actually turn brownish in color and vision will diminish more overtime along with color perception until blindness occurs (blindness is reversible with surgery, however).
Causes of Cataracts:
- Aging (senile cataracts)
- over time the lens starts to lose its transparency and proteins start to stick together on the lens and over time the lens becomes cloudy.
- Congenital
- born with a cataract
- example: mom had a rubella infection during 1st trimester
- Trauma to the eye
- Disease processes: diabetes (uncontrolled diabetes)
- Unprotected eye exposure to sunlight
- Medications: corticosteroids
- Lifestyle: smokers, alcohol consumption, family history
Signs and Symptoms of Cataracts
Not painful and happens gradually
CATS (remember the picture of the cat above)
Cloudy/blurry vision (can also have double vision in the affected eye)
Acquiring frequent eye glass prescriptions to help vision
Toned-down colors (washed out and faded)
Sensitivity to glare and light
- Lights seem too bright (glare) and halos around lights (tends to be worst at night…many patients notice this when they drive at night)
Tools Used to Diagnose Cataracts
If a cataract is severe enough, it can be easily visualized in the eye like the photo below: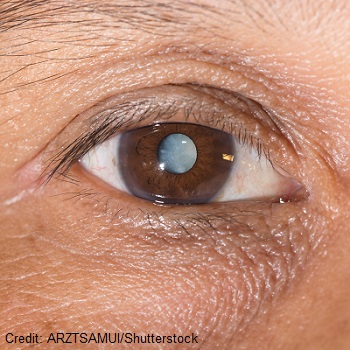
Ophthalmologist will perform a thorough eye exam such as:
- Visual Acuity test with Snellen Chart
- Slit-lamp: helps enlarge the front areas of the eye to allow the doctor to see the structures of the eye for evaluation like the cornea, lens, iris etc.
- Dilation of the pupils to assess the optic nerve with an ophthalmoscope
Cataracts Treatment
Monitoring the cataract until it progresses to a point where the patient cannot perform normal activities (first option)
- Regular eye checkups and changing eye glass prescriptions
- Anti-glare glasses
- Education: Protecting eyes from sunrays, magnifying items for better views, and adding more light
Surgery: remove the cloudy lens and replace it with an intraocular len (IOL)
Phacoemulsification: type of extracapsular extraction that is performed to remove the cloudy lens by breaking it up with sound waves. The old lens is removed and a new lens called an intraocular lens (IOL) is placed in the eye. This lens will stay in the eye permanently and is the eye’s new lens.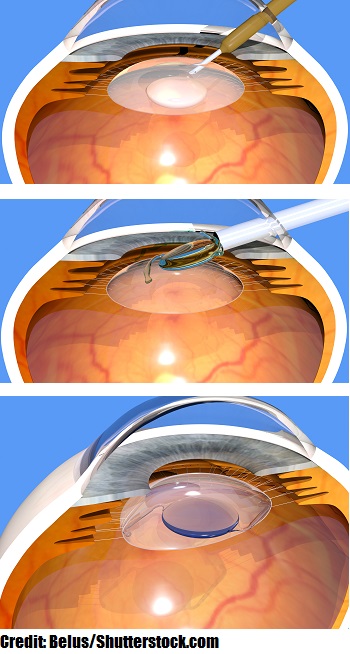
Nursing Interventions for Cataracts
Educate about Prevention
- Identify patients who are at risk and remember many patients develop cataracts when older…so the goal is to start early with preventive measures
LENS
Layers of protection: sunglasses that have UVA and UVB protection and large brim hats
Eat fruits and vegetables in diet
- They provide nutrients like vitamin C, E, lutein, zeaxanthin, which are all important for eye health. If diabetic educate about managing blood glucose levels.
No smoking (reduce alcohol consumption)
Schedule regular eye exams to monitor the health of the eyes
Surgery Interventions:
Before: Outpatient procedure and the procedure itself is quick (less than 15-20 minutes) and then patient is monitored in recovery and then goes home. One eye is treated at a time and the other eye will be treated at another time.
- NPO
- Driver to go home
- Eye drops before the surgery (some surgeons require the patient start instilling the eye drops 3 days before the procedure)
- Anti-inflammatory and Antibiotics
- Key education points for the patient:
- instill in the eye that is having surgery
- educate about waiting 3-5 minutes before instilling the other type of eye drop medication so it gives the eye enough time to absorb the first medication
- eye drop sequence typically does not matter
- demonstrate how to instill the eye drops in the conjunctival sac of the eye
- how to perform punctual occlusion to prevent the medication from absorbing in the systemic circulation
- Examples of eye medications used:
- Difluprednate (corticosteroid)
- Nepafenac (NSAID)
- Moxifloxacin (Antibiotic)
- Pre-op dilation of pupil needed right before surgery which the nurse may administer
- Why? The pupil must be dilated so the surgeon can obtain the best view of the eye when replacing the lens.
- Things to Remember:
- Patients with darker eye colors (like dark brown) may need higher doses of dilation medications to achieve the same effects compared to someone with blue, green eyes (these eye colors will dilate faster than people with dark brown eyes).
- Why? Dark brown eyes have more pigment (melanin) in them and the pigment binds or bounds the drops so people with a lot of pigment in the eyes need high doses (takes long to dilate).
- Lower the lights (makes eyes more sensitive to light) and blurry vision (will need assistance in getting up and moving around)
- Things to Remember:
- Assess if taking Tamsulosin (Flomax) or other types of alpha blockers
- These medications relax smooth muscle and can affect the iris and make it “floppy” (alters pupil dilation…remember the pupil needs to dilate for a successful surgery)
- Can lead to a condition called: intraoperative floppy iris syndrome…eye doctor must be aware prior to surgery
- Tamsulosin is used in men to treated an enlarged prostate.
- Examples of Pupil Dilation Medications:
- Mydriatics (Phenylephrine): works on the alpha adrenergic receptors of the eye and causes the iris dilator muscle to contract and when this occurs the pupil increases in size.
- Cycloplegics: paralyzes the ciliary muscle of the eye which results in the loss of accommodation.
- Why? The pupil must be dilated so the surgeon can obtain the best view of the eye when replacing the lens.
After Surgery:
- Position on non-surgical side.
- Eye shield worn after surgery (per surgeon recommendations and when removed wear glasses throughout the day)
- while sleeping or napping wear the eye shield to protect the eye from rubbing or trauma
- Eye drops needed (antibiotics, anti-inflammatory)….use clean hands
- Restricting activities that could increase eye pressure (heavy lifting, running, coughing, bending, swimming)…can watch TV as desired.
- Pain should be minimal (Acetaminophen if needed)
- Normal: itching (don’t rub) and blurriness normal for few day
- ABNORMAL: notify if severe pain or further decrease in vision, light flashes or floaters (could indicate retinal detachment), purulent drainage, excessive redness, or fever
- Keep appointments, will check eye healing (may need new glass prescription once healing process is over)
References:
Cataracts | National Eye Institute. (2019). Retrieved 11 July 2021, from https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/cataracts
Keep an Eye on Your Vision Health. Retrieved 10 July 2021, from https://www.cdc.gov/visionhealth/resources/features/keep-eye-on-vision-health.html
How the Eyes Work | National Eye Institute. Retrieved 15 July 2021, from https://www.nei.nih.gov/learn-about-eye-health/healthy-vision/how-eyes-work