Sinus tachycardia ECG heart rhythm review for nursing students!
In this review you will learn how to identify the cardiac rhythm known as sinus tachycardia. After this review you should be familiar with the following about this heart rhythm:
ECG criteria for tachycardia
Causes
Complications
Nursing interventions
Treatment
After you review this material don’t forget to watch the lecture on sinus tachycardia and to test your knowledge with this sinus tachycardia quiz.
Sinus Tachycardia ECG Review
Let’s break down the words:
Sinus: it’s a sinus type rhythm (meaning it’s originating from the SA node)
Tachy: fast or rapid cardia: the heart’s action
Meaning: it’s a heart rhythm that arises from the SA node that causes rapid heart action (hence a fast rate) that is regular
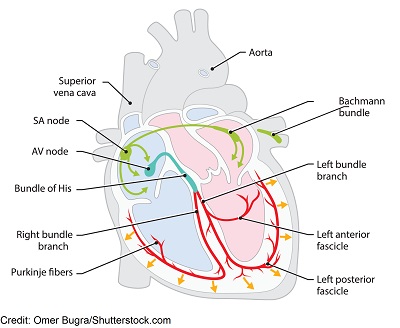
First, let’s talk about the SA node:
This node is found in the upper part of the right atrium. It’s known as the pacemaker of the heart and normally keeps the heart beating at a rate between 60-100 bpm.
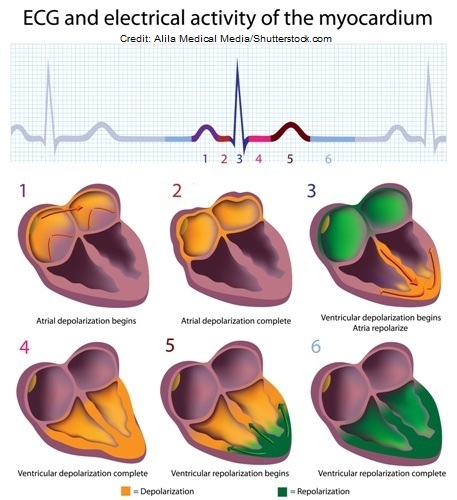
The SA node is the starting point for how the electrical signals travel down through the electrical conduction system of the heart. The electrical signal should start in the SA node, travel down through the internodals pathways, to the AV node, bundle of His, bundle branches, and then the purkinje fibers. This whole process creates the PQRST ECG waveform observed on an ECG strip.
If the SA node is sending out electrical signals like it should, it will create normal sinus rhythm on the ECG. However, if the SA node is firing rapidly it creates a rate of greater than 100 bpm to generally no faster than 160-180 bpm. This rhythm is referred to as sinus tachycardia.
In contrast, if the SA node is firing slowly at a rate of less than 60 bpm that is referred to as sinus bradycardia.
ECG/EKG Study Guide and Workbook for Nursing Students
“ECG/EKG Interpretation Study Guide and Workbook by Nurse Sarah”. This book contain 100 pages of content featuring 26 ECG rhythm break downs, 51 ECG rhythm analysis practice problems, 100 comprehensive ECG practice questions, worksheets, chart summaries, and more.
You can get an eBook version here: “Nurse Sarah ECG Book” or a physical copy here: “ECG/EKG Interpretation Study Guide by Nurse Sarah“.
Criteria for Sinus Tachycardia:
Sinus tachycardia meets the criteria of normal sinus rhythm but is FAST >100 bpm (to no more than 160-180 bpm):
- Normal p-waves (one in front of every QRS complex, round and upright)
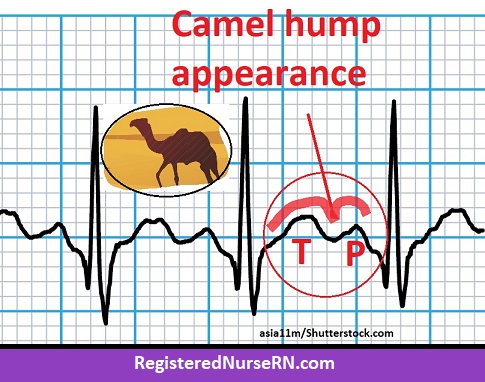
- **if the rate increases to 140-150s it may be hard to tell the p-wave and t-wave from each other because they are so close together, creating a “camel hump” appearance. In addition, the p wave can be slightly hidden or buried.
- Atrial and ventricular rates are regular but they are FAST >100 bpm
- Narrow QRS complex after every p-wave (<0.12 seconds)
- T-wave: after each QRS complex
- PR interval (normal 0.12-0.20 seconds)…if can measure if p-wave visible
- QT interval will be shorten (faster the heart the shorter the QT interval)
Analyze this rhythm:
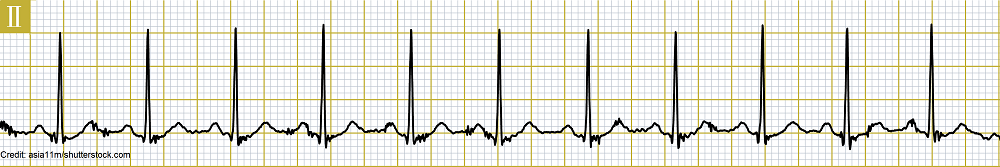
- P-waves: normal
- Atrial rate: 110 bpm
- Atrial rate: regular
- QRS complexes: normal
- Ventricular rate: 110 bpm
- Ventricular rate: regular
- QRS complex measures: 0.08 seconds
- PR interval: 0.12 seconds
- T wave: normal
- QT interval: normal
Interpretation: Sinus tachycardia with rate of 110 bpm
Causes of Sinus Tachycardia:
Sinus tachycardia *usually* occurs because the body needs oxygen. Therefore, the heart tries to compensate for that by increasing the heart rate. It hopes that by pumping faster it can get the oxygen the body needs to tissues and organs.
This occurs because something is triggering the SA node to fire rapidly. This trigger can be either related to an underlying disease or non-disease related. However, whatever the cause is, if it can be treated, removed, or corrected the sinus tachycardia will disappear and the heart rate should return to normal.
For example, exercise causes sinus tachycardia. When exercise ceases the heart rate drops and returns back to normal sinus rhythm. Or if a patient has anemia sinus tachycardia can occur. This is because the amount of red blood cells is reduced which limits the amount of oxygen available in the body and leads to sinus tachycardia.
One thing the nurse wants to keep in mind is that if a patient has an underlying medical condition, sinus tachycardia could present as a warning sign that the underlying medical condition is worsening and should not be ignored.
Therefore, if you have a patient who has had a recent heart attack or is experiencing blood clots (there is a high risk after surgery of a bone like the hips etc., postpartum period, immobile), and develops sinus tachycardia, you want to notify the physician.
With a heart attack it could mean your patient is developing cardiogenic shock. This is where the heart muscle was majorly damaged from the heart attack and is failing so the body is trying to compensate by increasing the rate but it is will fail.
Another example is with blood clots. If a blood clot breaks off and goes to the lungs (known as a pulmonary embolism) it causes oxygen demands to increase, pressures to alter, and increases the workload on the heart. This can lead to sinus tachycardia. If this happens also assess the patient for chest pain that worsens with breathing in, cough (example: contains blood) or shortness of breath.
To help you remember the main causes of sinus tachycardia, remember:
TACHY Hearts
Temperature elevation (infection leading to sepsis)…a fever increases oxygen needs of body
Aerobics (exercise)
Cardiac disease: congestive heart failure, myocardial infarction leading to cardiogenic shock
Hyperthyroidism (sinus tachycardia may be the only symptom for some patients)
Yelp! (pain)
Hemorrhage or hypovolemic shock
Emotional stress/fear
Anemia
Respiratory conditions: pulmonary embolism, pneumothorax, chronic lung diseases (oxygen decreased)
Therapeutics: atropine (anticholinergics), albuterol, dopamine, epinephrine
Stimulants: nicotine, alcohol, cocaine, caffeine, amphetamines
Problems or Consequences of Sinus Tachycardia
First of all, it’s not always a problem because with exercise it is a good thing to help us maintain heart healthy and burn calories. In fearful situations it can be beneficial in helping us escape danger. The sympathetic nervous system kicks into gear and increases the heart rate which helps prepare the body to fight.
But for some patients with underlying health problem (especially heart related like heart disease or weak heart function like heart failure) it can be deadly.
When the heart is beating fast, it is really placing a lot of stress on the heart muscle. In order to keep up, the heart muscle has to use a lot of oxygen so it can keep pumping at this rate. The oxygen is delivered to the heart muscle by coronary arteries.
Therefore, sitting on top of the heart muscle supplying it with all this oxygen are the coronary arteries. But if the patient has plaque or a blockage (hence coronary artery disease) in those arteries, it limits how much oxygenated blood can be delivered to the heart muscle.
If fatty plaques are limiting the blood flow, the heart muscle starts to become “ischemic” (it can die) and this causes the patient chest pain. This is why some patients may complain of chest pain when their heart rate rises. In turn, it could lead to a myocardial infraction.
In addition, if sinus tachycardia occurs for too long it can affect how well the heart can pump out blood. Fast rates of 150 or greater actually decrease how much blood the ventricles can pump out to the body. This is because the ventricles don’t have enough time to fill completely so less blood is pumped out. This leads to decreased cardiac output.
Signs of decreased cardiac output include: hypotension (<90 SBP) and signs of heart failure may develop: pulmonary edema (crackles), extra heart sounds), decreased level of consciousness, increase capillary refill time, cool extremities, etc.
Treatment and Nursing Interventions for Sinus Tachycardia
The goal is to identify the cause and treat it because this will decrease the rate.
Tests to assess: ECG, cardiac tests (stress test, echocardiogram), holter monitor, assess thyroid levels, blood levels (hemoglobin anemia, WBC infection), medication history
Medications to slow down the rate:
- Beta blockers: Metoprolol
- Calcium channel blockers: (Verapamil or Diltiazem)
- Miscellaneous: pain medication, antipyretics etc.
Nursing: ASSESS your patient for a potential cause (fever, pain, hemorrhage, and report it, monitor vitals and heart rhythm (assess for signs of decrease cardiac output: hypotension, confusion, syncope, decreased capillary refill time, shortness of breath, extremities are cool), administer medications per MD order, teach patient to avoid smoking, caffeine, and other stimulants.
References:
Henning A, Krawiec C. Sinus Tachycardia. 2021 Aug 11. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–. PMID: 31985921.
How the Heart Works | NHLBI, NIH. Retrieved 15 February 2022, from https://www.nhlbi.nih.gov/health-topics/how-heart-works
Sattar Y, Chhabra L. Electrocardiogram. [Updated 2021 Jul 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK549803/