This NCLEX review will discuss nephrotic syndrome vs glomerulonephritis.
As a nursing student, you must be familiar with nephrotic syndrome and acute glomerulonephritis along with how to care for patients who are experiencing these conditions.
These type of questions may be found on NCLEX and definitely on nursing lecture exams.
Don’t forget to take the nephrotic syndrome vs glomerulonephritis quiz.
You will learn the following from this NCLEX review:
- Definition of nephrotic syndrome vs glomerulonephritis
- Causes
- Pathophysiology
- Signs and Symptoms
- Nursing Interventions
NCLEX Lecture on Nephrotic Syndrome vs Glomerulonephritis
Nephrotic Syndrome vs Glomerulonephritis NCLEX Review
Nephrotic Syndrome
What is happening?
- Changes to the glomerulus of the nephron that leads to the leakage of a MASSIVE AMOUNT OF PROTEINS into the urine.

Main Causes:
- Changes to the glomeruli (cause not 100% known)
- Minimal change disease (most common cause) this disease shows glomeruli changes when assessed with an electron microscope
- Tends to affect the pediatric population (ages 2-5 years)
- Other causes can be secondary due to a disease causing changes to the glomeruli, such as lupus, diabetes, heart failure, etc.
Various types of proteins can be lost:
- Main protein lost is ALBUMIN…can also lose immunoglobulins that help fight infection and proteins that decrease clot formation.
Signs and Symptoms of Nephrotic Syndrome:
- Massive Proteinuria (>3 Grams per day)
- Foamy Frothy urine dark yellow
- Hypoalbuminemia (low levels of albumin in the blood)
- Hyperlipidemia: as the liver tries to make more albumin it will produce more triglycerides and cholesterol as well
- Edema: weight gain…starts in face and around the eyes and progresses to the extremities and abdomen
Main Nursing Concerns:
- Monitor fluid status and swelling (diuretics and IV albumin may be ordered by the physician to help with swelling and replace low albumin levels)
- At risk for infection (especially the edematous skin)
- Corticosteroids or immune suppressors to help decrease amounts of protein lost in urine…prevent relapse per physician’s order
- Assess for blood clots: deep vein thrombosis, respiratory change pulmonary embolism etc.
- Diet limiting sodium, potassium, fluid, and fat
- Educate about relapse and how to monitor for signs and symptoms
Acute Glomerulonephritis
What is happening?
- Inflammation of the glomerulus that leads to the leaking of RED BLOOD CELLS and PROTEIN (mild) into the urine.
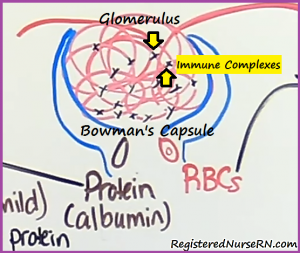
Main Cause:
- Post streptococcal infection
- (occurs 14 days after a strep infection of the throat or skin…impetigo)
- Tends to affect the pediatric population (ages 2-10)
Understanding how it works: AGN is not caused from the strep bacteria attacking the glomerulus but the immune system’s response to the bacteria by creating antigen-antibody complexes, which inflames the glomerulus. This is why you see it AFTER a strep infection.
Signs and Symptoms of AGN:
“Had Strep”
Hypertension
ASO antistreptolysin titer positive (test used to diagnose strep infections)
Decreased GFR: inflammation due to complexes in the glomerulus (low urine output)…oliguria (watch potassium level)
Swelling in face/eyes (edema)…mild
Tea-colored urine (cola colored)…from hematuria
Recent strep infection
Elevated BUN and creatinine
Proteinuria (mild)
Main Nursing Concerns:
- Monitor blood pressure (antihypertensive medications) and diuretics may be ordered by the physician.
- Monitor fluid status: intake and output…if oliguric watch for hyperkalemia because when the GFR is decreased potassium is not excreted properly, and swelling
- Diet limiting sodium and fluid…if oliguria presents will need to limit potassium-rich foods as well.
- Relapse not common but teach how to monitor for strep infections in the future and the importance of obtaining throat/skin cultures.
More NCLEX Reviews
References
- “Childhood Nephrotic Syndrome | NIDDK”. National Institute of Diabetes and Digestive and Kidney Diseases. N.p., 2014. Web. 20 June 2017.
- “Group A Strep | Post-Streptococcal Glomerulonephritis | | PSGN | GAS | CDC”. Cdc.gov. N.p., 2016. Web. 5 June 2017.