This nursing review will cover Systemic Lupus Erythematosus (SLE).
It is important the nurse is familiar with the pathophysiology of Lupus along with medications used to treat the condition, signs and symptoms, and patient education.
After studying this review about SLE, don’t forget to take the free Lupus NCLEX question quiz.
What is Systemic Lupus Erythematosus?
It’s an autoimmune condition (meaning the person’s immune system is attacking their own body) that causes inflammation to organs, joints, and tissues. This inflammation can eventually damage the affected structure permanently.
Where do these autoimmune attacks tend to occur (which parts of the body are affected)?
It’s important to note that the sign and symptoms that present in lupus are associated with the body system it affects, and this varies among patients. However, most patients with lupus will have at least one or more of these body systems affected.
Body Systems Affected by Lupus:
- Joints
- Lungs
- Skin
- Heart
- Brain
- Kidneys
- Blood System
Key Points about SLE:
- Systemic Lupus Erythematosus (SLE) is a chronic condition that has periods of flare-ups and remission.
- It takes investigative work to diagnose this disease because it’s presenting signs and symptoms are similar to other chronic diseases. Therefore, the patient’s family history, health history, presenting signs and symptoms, and lab results are all taken into account.
- Unfortunately, there is currently no cure at this time, but treatments are available to help patients go into remission and decrease flare-ups.
- There are different types of lupus and SLE is the most common type.
- It affects women more than men, specifically Black, Latina, Asian women in their child-bearing years.
- Therefore, it’s thought that hormones may play a role in this chronic disease because its onset correlates with menstruation and can become worst during pregnancy (flares).
What causes Lupus (Pathophysiology)?
Factors that could increase a patient’s risk for developing Lupus:
Family history (specific genes), environment (too much sun exposure, exposure to certain infections or medications), and hormones
Pathophysiology of Lupus
The patho of Lupus may be related to how a cell undergoes the death process. This process is known as apoptosis.
This process may not be occurring as it should be. This leads to an immune system attack, and the creation of antinuclear antibodies. These antinuclear antibodies are formed because the immune system sees the proteins found in the nucleus of the cells as nuclear antigens.
Now let’s look at this process in detail so you can get a better understanding of it.
Quick Review of the Cell
The cell consists of many parts. It has a cell wall on the outside, and on the inside it has many important structures such as the nucleus. The nucleus stores chromosomes with our DNA and plays an important role with synthesis of proteins and ribosomes.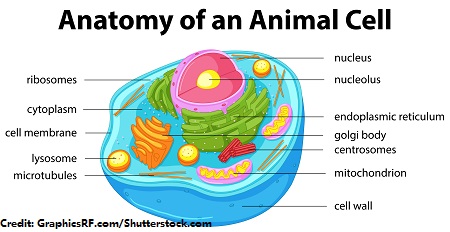
Our body has a process to keep our cells healthy and wants to prevent them from turning into cancerous or unhealthy cells that will kill us.
Therefore, when a cell gets sick, it knows it’s time to die because it doesn’t want to stick around and infect others by multiplying and growing. In turn, it starts to undergo apoptosis. This process must occur in a very specific sequence and within a proper time frame to prevent any complications.
Review of Apoptosis
Goal of Apoptosis: To get the sick cell and it’s inside material such as the nucleus, “consumed” by a team member of the immune system call the macrophages. The cell undergoes the following process:
- The cell decreases in size and the outer membrane loses it integrity and blebbing occurs.
- The inside contents of the cell, such as the nucleus and other cell structures in the cell break down. During this time, the cell has begun to signal to the macrophages to come clean up, hence “eat”.
- Then the cell begins to shatter into tiny pieces and forms apoptotic bodies.
- At this point, the macrophages arrive to the scene to engulf these pieces (this process is called phagocytosis). Then, the process is complete.
****In patients with lupus, the phagocytosis process is too slow and/or performed incorrectly. In turn, apoptotic bodies are not consumed efficiently. These bodies breakdown and leak cell material into the body. Remember in these bodies are nuclear material (DNA) from inside the cell. Once it is leaked, it enters the extracellular space and is detected by the immune system that will see it as a foreign invader (hence antigens, specifically nuclear antigens) that must be destroyed.
Therefore, the immune system creates antinuclear antibodies that attack the nuclear antigens. When attacked this forms an immune complex. These immune complexes float around in the blood and can get stuck in the basement membranes of capillaries that made up our kidneys and other structures etc.
The presence of these immune complexes activates the complement cascade. This system consists of special proteins that have a job to “complement” or to promote the role of the immune system to fight foreign invaders by promoting inflammation. However, this complement system isn’t helping fight a foreign invader, but the patient’s own cell material that the body has mistakenly decided was a foreign invader. Therefore, healthy cells of that structure die, and this is why we start to see healthy systems malfunction.
Signs and Symptoms of Systemic Lupus Erythematous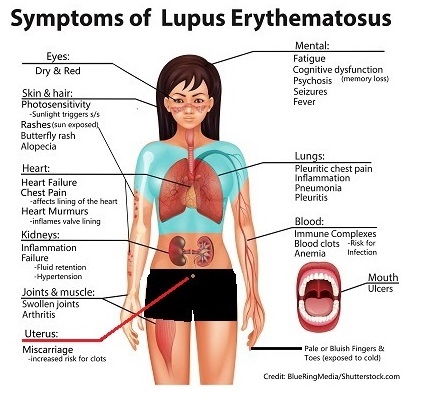
Signs and symptoms in lupus occur as “flare-ups” and then go into remission. It’s important the patient is aware of possible triggers and early signs/symptoms of a flare.
Signs and symptoms also vary among patients. This is because it depends on where the immune complexes are congregating to affect the healthy cells of that organ, joint, or tissue (remember that lupus can affect any body system).
Nurse’s Role in Systemic Lupus Erythematosus
LUPUS
Labs to help diagnose and monitor flares
- Antibody Labs:
- Positive ANA (anti-nuclear antibodies): if positive, this demonstrates there are autoantibodies the body created against the nuclei of the cell (almost all patients with lupus will have a positive ANA, but these anti-nuclear antibodies can also be present with other autoimmune disorders).
- Anti-dsDNA (anti-double stranded DNA anti-body): this is a particular antinuclear antibody found in some patients with lupus and is not typically present in patients who don’t have lupus.
- Anti-Sm antibody (Anti-Smith antibody): particular antibody found in the nucleus that correlates with lupus.
- Elevated ESR (erythrocyte sedimentation rate) and CRP (c-reactive protein): monitors inflammation in the body and helpful with detecting lupus flares and if treatment is working (not specific just for lupus because other disease processes can cause inflammation).
- Complement test (proteins C3 and C4)….low count: assesses if inflammation is occurring, and if these proteins are being used in this process of inflammation. A decreased amount shows this system is active and using up proteins to cause inflammation.
- CBC, metabolic panel etc.
Use Medications: to decrease occurrence of flares, protect organs/tissues/joints from damage, and improve quality of live.
Steroids: Prednisone, Prednisolone etc.
- Decreases inflammation quickly, but causes side effects
- Used when patient is not experiencing relief from other medications (severe cases)
- Not for long-term usage and must be tapered off
- Side Effects: weight gain, diabetes, osteoporosis and increased risk for infection
NSAIDs (non-steroidal anti-inflammatory drugs): Ibuprofen, Naproxen etc.
- Decreases inflammation (helpful with fever, joint pain)
- GI issues (risk for ulcers and bleeding), take with food, and can affect kidney function
Antimalarial: Hydroxychloroquine (very common med for patients with severe lupus)
- Decreases antibodies attacking the body, helps control the disease long term (preventing flares)
- Doesn’t work immediately (takes couple of months)
- Take with food to prevent GI problems
- Must have eyes checked regularly if taking long-term (minimum yearly) to monitor the retina
- No smoking (makes drug less effective)
Immunosuppressant: Azathioprine or Mycophenolate Mofetil etc.
- Suppresses immune system (increases risk for infection and certain cancers)
- For severe cases of lupus and sometimes you may hear them referred to as “steroid-sparing” meaning the use of them helps lower the amount of steroids the patient may have to take. Remember steroids can cause adverse side effects.
- Educate about preventing infection and monitoring self for infection because the medication regime for lupus (example: taking steroids as well) can prevent the signs and symptoms of infection appearing (example: fever).
- Vaccines up-to-date but no live vaccines (shingles, MMR, intranasal flu, smallpox, rotavirus)
Biologics: Belimumab
- Binds with a protein that supports the activity of B-cells to decrease the activity of B-cells…result: decreases antibody attacks and decreases inflammation
- Take with other lupus medications
- Takes time to start experiencing relief (half a year)
- Infusion or injection (subcutaneous)…fat of the upper thighs or abdomen
- Assess mental health
- Risk for depression (trouble sleeping, loss of appetite, loss of interest, sadness, etc.)
- Suicidal thoughts
- Monitor for infection
- No LIVE vaccines
Pregnancy (many patients are childbearing age and need education):
Women who want to become pregnant need to make sure their lupus has been in control for at least 6 months before conceiving. Pregnancy and the post-partum period can cause flares.
Understanding Flares
Triggers: sunlight, stress, sickness, not taking medications correctly or needing an adjustment
Prevention: “LESS” Flares
- Lower stress (avoid overworking, emotional, illness, and use techniques to help prevent stress)
- Exercise (helps joints and manages weight)
- Sleep (need more than 8 hours to prevent the body from getting too exhausted)
- Sun Protection (sunscreen and large-brimmed hats…sunlight can activate a flare)
Signs of a flare of lupus: educate patient to keep diary of symptoms to monitor for flares
- Fatigue
- Low grade fever
- Achy joints
- Rash
- Edema of the legs and hands
References:
Huang, W. N., Tso, T. K., Wu, H. C., Yang, H. F., & Tsay, G. J. (2016). Impaired phagocytosis of apoptotic cell material in serologically active clinically quiescent patients with systemic lupus erythematosis. International journal of rheumatic diseases, 19(12), 1310–1316. https://doi.org/10.1111/1756-185X.12826
Lupus Therapies Continue to Evolve. U.S. Food and Drug Administration. (2021). Retrieved 4 October 2021, from https://www.fda.gov/consumers/consumer-updates/lupus-therapies-continue-evolve.
Pregnancy and Lupus. Office on Women’s Health (OASH). (2018). Retrieved 4 October 2021, from https://www.womenshealth.gov/lupus/pregnancy-and-lupus.
Systemic Lupus Erythematosus (SLE). Cdc.gov. (2018). Retrieved 4 October 2021, from https://www.cdc.gov/lupus/facts/detailed.html#sle.