Learn about cardiac preload and afterload in this cardiovascular NCLEX review for nursing students!
Why is it important to know about preload and afterload as a nurse? These two concepts influence cardiac output because they both play a role in stroke volume.
Cardiac output is the amount of blood the heart pumps per minute. The heart pumps about 4-8 liters of blood per minute, which provides oxygen to our organs and tissues.
Therefore, CO plays a huge role in tissue perfusion. If cardiac output falls too low, tissue perfusion is diminished to the cells that make up our tissues and organs. When tissue perfusion is decreased, cells don’t receive enough oxygen and will start to die. We discussed how cells are affected by low cardiac output in our review on the stages of shock.
Cardiac output is calculated by taking the heart rate and multiplying it by stroke volume.
CO = HR x SV
Lecture on Preload and Afterload
Let’s talk about stroke volume:
Stroke volume is the amount of blood pumped by a ventricle with each beat. Stroke volume is affected by three factors:
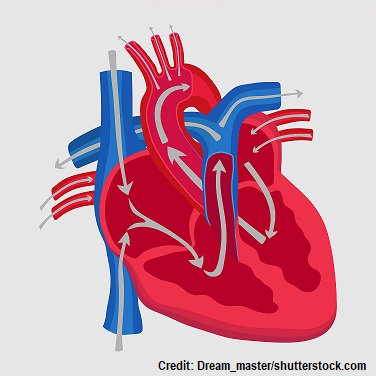 Preload, afterload, and contractility
Preload, afterload, and contractility
Contractility is the strength of the heart’s cells to shorten or contract.
Preload is the amount the ventricles stretch at the end of diastole. Diastole is the filling or relaxation phase of the heart. In other words, preload is the volume that has FILLED the ventricles at the end of the filling phase for the ventricles. Preload is also called the end-diastolic volume (EDV).
Preload can be manipulated to help with increasing stroke volume, which will help increase cardiac output.
What can increase cardiac preload? IV fluids, sympathetic nervous system stimulation (leads to vasoconstriction…this can occur naturally through the fight or flight response system or via medications called Vasopressors)
Reasons for increasing cardiac preload? One situation would be when a patient is in hypovolemic shock. In hypovolemic shock, a patient’s fluid volume in the intravascular space is very low and this leaves the heart very little to pump. The preload can be increased by administering intravenous (IV) fluids.
IV fluids will increase preload by adding more fluid volume to the venous system. This will increase the venous return to the heart. The extra fluid will fill the ventricles and increase the stretch of the ventricle at the end of diastole due to the extra fluid volume.
Sympathetic nervous system stimulation can increase preload too. The vasoconstriction that occurs with SNS stimulation causes vessels to narrow throughout the body and this will increase blood return to the heart…hence preload.
What can decrease cardiac preload? Diuretics (example: Furosemide), vasodilation
Reason for decreasing cardiac preload? When a patient is presenting with congestive heart failure there is a back up of fluid in the heart that will back flow to the lungs. This increases the workload on the ventricles due to the extra blood volume. Diuretics can be given to remove that extra blood volume and this will decrease the venous return to the heart, which will decrease preload (it will decrease the amount the ventricles stretch at the end of its filling phase).
In addition, vasodilators (example: Nitroglycerin) can decrease preload. These medications will dilate vessels and this will lead to pooling of blood, which will decrease the venous return to the heart. Again, this will decrease the amount of blood that fills the ventricles at the end of diastole.
Afterload is the pressure the ventricles must work against to open the semilunar valves and pump blood out of the heart.
However, to do this the ventricles must overcome VASCULAR RESISTANCE. This vascular resistance comes from either the lungs (known as pulmonary vascular resistance and deals with the right ventricle ) or the body’s circulation (known as systemic vascular resistance and deals with the left ventricle).
If the resistance is high, this will increase the afterload. If resistance is low, it will decrease the afterload.
Let’s talk about this further:
Pulmonary vascular resistance (PVR): The right ventricle’s goal is to pump blood to the lungs so the blood can become oxygenated. To do this, the right ventricle squeezes blood through the pulmonic valve (a semilunar valve) to the pulmonary artery, which takes it to the lungs.
In order to do this successfully, the right ventricle must OVERCOME the pressure in the pulmonary artery (hence the pulmonary vascular resistance) to open the pulmonic valve so blood can leave the ventricle and go to the lungs. If pulmonary vascular resistance is HIGH, the right ventricle will have an increased pressure it must work against to open the pulmonic valve…hence it will have an INCREASED afterload.
Systemic vascular resistance (SVR): This can also be applied to the left ventricle as well. The left ventricle’s goal is to take fresh oxygenated blood and pump it through the aortic valve and to the aorta. The aorta will take the blood to the body.
In order to do this successfully, the left ventricle must OVERCOME the pressure in the aorta (hence the systemic vascular resistance) to open the aortic valve so blood can leave the ventricle and go to the body. If systemic vascular resistance is HIGH, the left ventricle will have an increased pressure it must work against to open the aortic valve…hence it will have an INCREASED afterload.
What can increase cardiac afterload?
Vasoconstriction: this will cause narrowing of vessels in the body and increase blood pressure. This will increase vascular resistance and the pressure the ventricle must work against to open the semilunar valves so blood can leave the ventricle. An example of this would be the administration of vasopressors or pulmonary hypertension (this condition increases pulmonary vascular resistance).
Valve issues: example aortic stenosis. This is narrowing of the aortic valve, which will lead to an obstruction of outflow of blood. It will make it hard for the ventricle to pump blood out of the valve….hence increase afterload.
What can decrease cardiac afterload?
Vasodilation: this will widen vessels and decrease vascular resistance…hence decreasing cardiac afterload.
Test your knowledge: preload vs afterload quiz