This NCLEX review will discuss pressure injuries (formerly called pressure ulcers).
As a nursing student, you must be familiar with pressure injuries and how they affect our patients. In addition to the various stages, nursing interventions, and treatments for pressure injuries.
Don’t forget to take the free pressure injury quiz after reviewing this material.
Lecture on Pressure Injuries
Pressure Injuries NCLEX Review
Pressure Injuries: formerly called pressure ulcers and have been previously called decubitus ulcers and bedsores as well.
What is a pressure injury? It is the breakdown of skin integrity due to unrelieved pressure of some type.
Unrelieved pressure can be from a bony area on the body that comes into contact with a hard surface or a medical device that causes unrelieved pressure (nasal cannula, bed pan, ortho device…splints etc.). In addition, this can happen due to friction and shearing of the skin. This is where the skin and bone are pulled in opposite directions causing injury to the capillary bed that perfuses the skin.
How do pressure injuries happen?
Example: Let’s say a patient is sitting in a bedside chair for a long time and can’t shift their own weight without assistance. What bony prominence is a great site for a pressure injury to develop in this position? Coccyx bone!
The exerted pressure from a bony prominence and in this case it is the coccyx bone, and the external surface (hence the chair’s seat) leads to a decrease in the blood supply to the epidermis and dermis. HOW? As the bone pushes down and the external surface pushes up it pinches the blood supply shut. This leads to a decrease in blood flow to the skin layers and the potential development of a pressure injury.
Risk Factors for Pressure Injury Development
Risk Factors: think of any patient population that has issues with alleviating pressure on a bony prominence (can’t verbalized it to you or move themselves) or will have issues with skin integrity
- Poor Nutrition….decreases skin integrity
- Immobile….can’t alleviate pressure
- Neuro Issues: unaware of the need to shift weight….spinal cord injuries or altered mental status….can’t alleviate pressure
- Diabetics….decreased awareness with sensory (decreased ability to feel pain due to nerve damage) and decreased circulation
- Incontinence of urine or stool….decreases skin integrity
- Activities that cause friction and shear….patient sliding down in the bed or not properly moved up in the bed etc.
Top Sites from Pressure Injuries (be aware of your patient’s position)

- Heels and Ankles
- Hips
- Sacral
- Elbow
- Shoulder
- Inside of the knee
- Occipital (back of head) and Ears
Staging of Pressure Injuries: based on National Pressure Injury Staging System

Stage 1: Skin is completely intact! The area will be very red but it does NOT blanch (hence turn white when pressed on).

Stage 2: Skin is visibly damaged and NOT intact with PARTIAL loss of the dermis. No subq (fatty tissue) will be visible. Wound may be opened with superficial red/pink opened ulcer or may have the formation of an opened or closed blister.
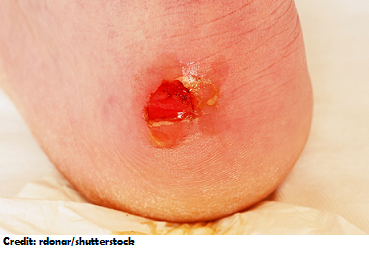
Stage 3: Skin is visibly damaged and NOT intact with FULL loss of the skin tissue. May see the subq (fatty tissue). Wound edges may be “rolled” away…..epibole. Bone, tendon and muscle NOT visible.
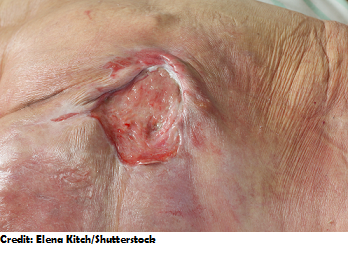
Stage 4: Skin is visibly damaged with FULL loss of the skin tissue that will expose bone, muscle, tendon, and ligaments.

Unstageable:
Slough (yellowish or tan) or eschar (brownish black) is covering a full thickness ulcer. You can’t assess the actual depth of the wound because of the slough or eschar covering the ulcer.
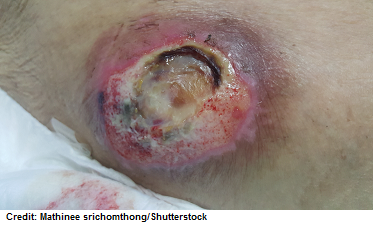
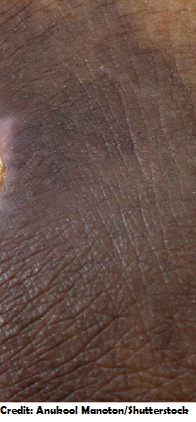
Deep-Tissue Injury:
Presents as purplish or blackish areas over skin that is intact. The fatty tissue below is injured. Also, may look like a black blister area. It may feel heavy or spongy.
(“NPUAP Pressure Injury Stages | The National Pressure Ulcer Advisory Panel – NPUAP”, n.d.)
Nursing Interventions for Pressure Injuries
PREVENTION! DETECTION! Wound Care!!
Prevention!
On admission: Assess from head-to-toe for any types of pressure ulcers, especially over bony prominences and document it thoroughly…..stage, size, color, drainage….notify physician of the wound….may need order to consult wound care team or for a wound culture if an opened wound is present…..may contain MRSA or other antibiotic resistant bacteria etc.
Assess for potential patients who are at most risk for pressure injuries using the Braden scale every shift:
It has 6 categories:
- sensory, moisture, activity, mobility, nutrition, and friction and shear
- 9 or less: Very high risk of developing a pressure injuries
- 19-23: No risk
Keep skin dry and clean on patients with incontinent issues (barrier creams to protect skin) or who are sweaty.
Make sure the patient has clean linens and is always wearing a clean gown….try to use articles that are wrinkle free.
Turn every 2 hours…the minimum of how often a patient should be turned.
Watch for friction and shear activities….be careful moving up in the bed.
- When patient is sitting up, position the bed so they can’t easily slide down. HOW? Slightly elevate the foot of the bed. Also, take special care when moving the patient up in bed. Use a transfer pad and lift the patient up….don’t scoot them up.
Be aware there are special air beds for patients at major risk for pressure injuries. In addition, there are heel boots, elbow pads, and gel cushions (especially if the patient uses the wheelchair often or sits in the beside chair a lot)…these are just a few items available to help prevent pressure injuries.
Routinely assess the skin integrity that comes into contact with medical devices.
Recommend a nutrition consult: this can help improve the patient’s diet to promote wound healing.
Wound care per wound care nurse recommendations: the wound care nurse will assess the wound and write out a plan of care for the nurse to follow. This usually includes specific types of dressing changes based on the severity of the injury (products to be used) and how often to change the dressing.
There are various methods for treating a pressure injury and it depends on the severity and stage of the injury: wound vac, debridement of the wound, dressing changes, hyperbaric oxygen therapy (high amounts of oxygen delivered to the wound to promote healing) etc.
References:
NPUAP Pressure Injury Stages | The National Pressure Ulcer Advisory Panel – NPUAP. Npuap.org. Retrieved 26 February 2018, from http://www.npuap.org/resources/educational-and-clinical-resources/npuap-pressure-injury-stages/
Pressure Sores | Bedsores | Pressure Ulcers | MedlinePlus. Medlineplus.gov. Retrieved 26 February 2018, from https://medlineplus.gov/pressuresores.html