Guillain-Barré syndrome NCLEX review for nursing students. This review is part of a neuro review, so be sure to check out those other NCLEX reviews.
Don’t forget to take the quiz that contains Guillain-Barré syndrome NCLEX questions.
Lecture on Guillain-Barré Syndrome
Guillain-Barré Syndrome NCLEX Review
What is Guillain-Barré syndrome? It’s an autoimmune neuro condition where the immune system attacks the nerves in the peripheral nervous system and cranial nerves.
What specifically is the immune system attacking? The immune system, which was attacking the illness (see more about this below), starts to confuse the cranial and PNS nerves for the illness. Therefore, the immune system begins to attack the myelin sheath (demyelination occurs) on the nerve cell.
Remember the role of the myelin sheath? This structure helps with nerve transmission. The myelin sheath normally functions as an insulator to help nerve transmission. The myelin sheath are very helpful structures that unfortunately become attacked by the immune system, and when this occurs it leads to a decrease or complete absence in nerve signaling.
Why is this happening? It is important to remember that GBS can happen to any person at any age! There is currently no cure, but treatment can help decrease signs and symptoms if started within 2 weeks of symptoms.
With GBS, a previous infection usually has started it all! Many patients will start to have signs and symptoms of Guillain-Barré syndrome about 1-2 weeks AFTER some type of viral or bacterial infection or one of the following:
So, as a nurse always complete a thorough health history:
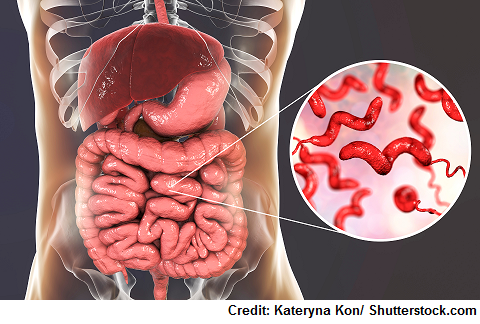 Recent upper respiratory illness or gastrointestinal infection (especially Campylobacter jejuni)
Recent upper respiratory illness or gastrointestinal infection (especially Campylobacter jejuni)
- An interesting statistic by CDC.gov, “As many as 40% of GBS cases in the United States are thought to be triggered by Campylobacter.”
- Vaccine (swine flu etc.)
- Surgery
- Epstein-Barr virus HIV/AIDS, flu infection
Various types of Guillain-Barré syndrome:
Cases can vary from mild to very severe.
- Acute inflammatory demyelinating polyneuropathy (AIDP): most common type in the US and what we will concentrate on in this lecture. It starts with paralysis/weakness/tingling sensation in the LOWER EXTREMIES (symmetrically) and migrates upward over time. It can be so severe the person will experience paralysis.
Mnemonic for Guillain-Barré syndrome: “GBS”
- Gradual
- Blocking of
- Sensation
There is another type called: Miller Fisher Syndrome. Eye paralysis is usually the first sign and symptom with this type.
What is happening in GBS?
 GBS: Gradual Block of Sensation
GBS: Gradual Block of Sensation
Let’s talk Nerves (which helps explain signs and symptoms)
Peripheral nervous system nerves are involved! Therefore, we’re talking about all the nerves outside the brain and spinal cord.
The PNS creates a connection between our brain/spinal cord to the rest of our body (so our limbs, muscle, and some of the organs are involved). AIDP is the most common type of GBS in the U.S.
Most patients start to have this weird tingling or numbness sensation (PARAESTHESIA) in their feet, which will gradually spread upward (symmetrically). Paralysis, absent reflexes, and loss of muscle tone is likely to follow the paresthesia.
As a side note: It’s very important to note that GBS PEAKS in about 2 weeks with its severity of symptoms, and then slowly recovery occurs (remylenation of the myelin sheath). Nurse: reassure the patient and always communicate with them because patients who experience GBS are extremely fearful.
In addition, it takes about 1-2 years for the patient to return to baseline (most patients have to complete some type of physical rehab after experiencing GBS due to the complications associated with it in regards to muscle atrophy and nerve damage).
As the demyelination spreads, it can start to affect the autonomic nervous system of the PNS. Remember the PNS can be separated into the somatic nervous system (controls voluntary movement functions) and autonomic nervous system (involuntary functions).
***In severe cases of GBS, the autonomic system (parasympathetic and sympathetic nervous system) can be affected. Therefore, we’re talking about the nerves that regulate our blood pressure, heart rate/rhythm, temperature, vision, GI (constipation… decrease in motility of the GI system) and renal (retention of urine due to sphincter issues).
Signs and Symptoms associated with autonomic dysfunction:
- Inability to regulate body temperature
- blood pressure issues (orthostatic hypotension and paroxysmal hypertension)
- cardiac dysrhythmias
Cranial nerves: In addition, there can be cranial nerve involvement, as it gradually migrates up to the area of the brain stem where the cranial nerves are located. This leads to vision problems, paralysis of the face, issues swallowing, trouble speaking etc.
Let’s look at a typical scenario: A patient is 35 years old and has no pertinent information in their health history other than that they were sick about 2 weeks ago with a GI illness. However, they’ve recovered from it but now are presenting with this tingling, numbness, and weakness in the feet (called paresthesia) and it’s making walking difficult. They tell you they haven’t injuried themselves and the sensation is getting worst.
This is how some patients may present with GBS (but this syndrome is just starting).
As time goes on, you will find that these signs and symptoms start to migrate up and are symmetrical in origin. The patient’s reflexes will become majorly diminished or absent. This will affect the legs, arms, chest muscles used for breathing, face/eyes/swallowing ability (cranial nerves), and in severe cases the autonomic nervous system.
As more time goes on the signs and symptoms go from weakness to paralysis (ex: paralyzed from neck down), lose muscle tone, absent reflexes, facial paralysis, issues swallowing, talking, weak cough (need suctioning, short of breath, reports they can’t breathe in very well) and autonomic issues.
****Respiratory system is a major focus for the nurse!!! When this system is affected, most patients will need to be intubated or have a tracheostomy for assistance to breathe. Monitor for signs and symptoms that this system is being affected.
These signs and symptoms peak at about 2 weeks from when the symptoms started. Then slowly the signs and symptoms (remyelination of myelin sheath) start to resolve slowly. Most patients can make a full recovery within 1-2 years, but there are usually major complications afterwards due to paralysis that puts the patient on a long road to recovery.
One important thing to point out that although the patient is experiencing paralysis or weakness, many patients will experience severe pain like muscle pain/ cramps. Exact reason not known….may be due to nerve damage. But it’s very important as the nurse to evaluate the patient for pain using some type of communication technique.
However, because of severity of the muscle weakness most patients end up needing to be intubated (as stated above), develop infection (pneumonia from aspiration or ventilator acquired), at risk for blood clots and pressure injuries due to immobility, severe weight loss from nutrition issues, and will need intense physical therapy.
How is Guillain-Barré syndrome Diagnosed?
- Electromyography and nerve conduction studies: assesses for demyelination of nerves by determining muscle’s ability to respond to nerve stimulation
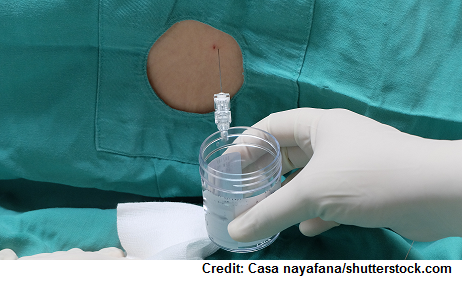
- Lumbar puncture: elevated protein without elevated white blood cells.
Nursing Role for Lumbar Puncture:
- Before: empty bladder
- During: position lateral recumbent with knees up to abdomen and chin to the chest
- Post: lay flat per MD order (helps decrease headache)…head not to be elevated, patient needs fluids to help replenish fluid taken (help decrease a headache as well)
Nursing Interventions for Guillain-Barré Syndrome
Focus: Respiratory, blood clots (immobility) risk for PE and DVTs, heart rhythm, blood pressure issues, nutrition, infection (urinary retention and lung from vent or pneumonia), pain, pressure injuries, atrophy of muscles, extreme fear
Collect a detailed health history
Monitor for progression of the syndrome and if the patient is getting worst:
- Spread of the paresthesia or paralysis?
- Change in reflexes?
- RESPIRATORY status (is it hard for the patient to talk, feel like they can’t breathe, can’t clear secretions, decrease respiratory rate, always having to suction patient?)
- Have airway management equipment at bedside
- Evaluate their swallowing…at risk for aspiration
- Communication….patient is aware but can’t communicate…use a white board
- Pain (severity and treat accordingly)
- Pressure injuries due to immobility: need frequent turning to prevent pressure injuries
- Prevent blood clots (SCDs, anticoagulants)
- Intake and output (may need catheter to drain urine due to urinary retention)
- Eye care due to facial paralysis (keep eyes moist with drops etc.)
- Nutrition: assess bowel sounds (at risk for paralytic ileus), constipation (decrease in gastric motility )and may experience an increase in gastric residuals so always check prior to a new feeding)….most patients will have a feeding tube
Management of airway with mechanical ventilation
Pain control
PT to work with and ROM to prevent muscle wasting and contractures
Keep patient informed (this is scary…you usually have a once healthy person now experiencing severe paralysis and can’t breathe on their own….make sure you have some way to communicate because they will most likely be aware of everything going on and reassure this is most likely temporary)
Treatments for Guillain-Barré syndrome
 Not a cure but helps speed up recovery: administered within 2 weeks from onset of symptoms….if greater than this time frame…doesn’t really help decrease signs and symptoms
Not a cure but helps speed up recovery: administered within 2 weeks from onset of symptoms….if greater than this time frame…doesn’t really help decrease signs and symptoms
- PLASMAPHERESIS: machine that will filter the blood to remove the antibodies from the plasma that are attacking the myelin sheath (help decrease signs and symptoms not a cure)
- Immunoglobulin therapy: IV immunoglobulin from a donor given to the patient to stop the antibodies that are damaging the nerves.
References:
- Guillain-Barré Syndrome Fact Sheet | National Institute of Neurological Disorders and Stroke. Retrieved from https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Guillain-Barr%C3%A9-Syndrome-Fact-Sheet
- Guillain-Barré Syndrome | Campylobacter | CDC. Retrieved from https://www.cdc.gov/campylobacter/guillain-barre.html