Glaucoma is a set of eye diseases that is caused by increased intraocular pressure (IOP) which damages the optic nerve.
The optic nerve transmits the visual surroundings we see from our eyes to the brain. If this nerve becomes damaged it results in vision loss and eventually blindness that will be permanent.
Don’t forget to take the quiz that contains glaucoma NCLEX questions.
Key Points about Glaucoma:
- No cure but there are treatments to help prevent damage to the optic nerve by lowering the IOP, hence prevent blindness.
- There are different types of glaucoma. We will talk about the two main types in this lecture called: open-angle and angle-closure
- Most common type is called open-angle, and the symptoms are very subtle with many people being unaware they have glaucoma until the disease has advanced.
- Angle-closure (also sometimes referred to as narrow-angle or closed-angle) is rare but develops suddenly and requires immediate intervention.
- Early detection is vital with glaucoma, which can be done with an eye exam to monitor intraocular pressure.
Pathophysiology of Glaucoma
The key players for understanding the patho of glaucoma are intraocular pressure and aqueous humour.
What’s intraocular pressure?
Intra means within and ocular means eye…so intraocular pressure is the fluid pressure within the eye, and the fluid we’re talking about is called aqueous humour. IOP is calculated by the production and drainage rate of aqueous humour in the eye. The production and drainage rate should be equal or increased intraocular pressure will occur.
A tonometer is used to measure the intraocular pressure. A normal intraocular pressure is about 10-21 mmHg.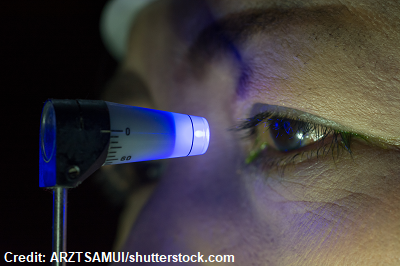
What’s Aqueous Humour?
It’s the fluid within the eye that has many roles, but it plays a significant role with maintaining intraocular pressure.
How aqueous humour is produced and flows through the eye helps us understand glaucoma. Therefore,first let’s discuss the normal flow of aqueous humour in the eye without glaucoma presenting:
Aqueous Humour Flow Path
Ciliary body produces aqueous humour-> the aqueous humour first goes through the posterior chamber of the eye which is found between the lens and iris-> then it goes through the pupil’s opening and makes its way to the anterior chamber, which is found between the iris and cornea -> then it drains out via the drainage angle into the trabecular meshwork (which is permeable and like a strainer) -> then into Schlemm’s canal and eventually into the episcleral veins of the eyes.
**An important area I want to talk about is the drainage angle. This area is where an angle is formed at the front of the eyes between the iris (the colored part of the eye) and cornea….hence this area forms an angle.
This angle is where aqueous humour drains out into the trabecular meshwork. It’s the angle we are talking about when we refer to either open or closed angle glaucoma. An ophthalmologist can check the patient’s drainage angle with a gonioscope.
Types of Glaucoma

Open-angle glaucoma:
In open angle glaucoma, the drainage angle is opened (so the angle between the cornea and iris is wide/opened like it should be) but the trabecular meshwork is clogged.
Why does it become clogged? As we get older the meshwork doesn’t work as well to drain aqueous humour and becomes thick and less permeable. Therefore, aqueous humour does not drain out but stays in the eye and increased intraocular pressure occurs. This pressure will compress the optic nerve, which overtime will cause vision loss.
Signs and Symptoms of Open-angle Glaucoma
- Silent: asymptomatic in early stages…you may have heard it referred to as a “thief of sight”
- It happens gradually and when the patient notices the s/s the disease has advanced to permanent vision loss.
- No pain
- Increased intraocular pressure (patient needs to have various readings at different times)
- Optic disc cupping: found when assessing the fundus of the eye with an ophthalmoscopy…looks at the optic disc to cup ratio.
- The optic disc is found on the fundus and in the middle of the disc is the optic cup. In chronic open-angle glaucoma the cup will enlarge and change the disc-cup ratio.
- Below is a picture of a normal optic nerve on the right…note the cup (bright part in the middle) is smaller than the disc but on the left the optic cup is a lot larger.

- Below is a picture of a normal optic nerve on the right…note the cup (bright part in the middle) is smaller than the disc but on the left the optic cup is a lot larger.
- Loss of peripheral vision: this is side vision (not really noticeable to the patient until they develop tunnel vision)….example here:

- The optic disc is found on the fundus and in the middle of the disc is the optic cup. In chronic open-angle glaucoma the cup will enlarge and change the disc-cup ratio.
Angle-closure glaucoma:
In angle-closure glaucoma the drainage angle becomes very narrow, hence closed (the drainage angle between the cornea and iris is closed/narrow). Therefore, aqueous humour can’t drain down into trabecular meshwork (which is functioning and NOT clogged). This type is rare but if it happens it is requires emergency treatment.
How the drainage angle becomes closed? Example: The iris or lens can become pushed forward which closes off the angle. This can happen with anatomical defect where the angles are already narrow, trauma to the eye, or pupil dilation through medications:
Anticholinergics: dilate the pupils…found in many medications like allergy, copd, depression medication etc.
Signs and Symptoms of Angle-closure glaucoma:
- Severe eye pain
- Nausea and vomiting
- Vision changes: blurred/seeing halos around lights
- Red eyes
- Edema of the cornea

- Increase intraocular pressure
Nursing Interventions Glaucoma
To help us remember key concepts about treatment, medications, education let’s remember the word:
“Thief”
Treatment goal is to reduce intraocular eye pressure to prevent damage to the optic nerve
- Medication first-line treatment (eye drops or oral meds) if don’t work may need
- Surgical (laser procedure or general traditional eye surgery)
Selective Laser Trabeculoplasty (SLT): quick procedure that is completed in minutes. It lowers IOP by using lasers to target certain parts of the drainage angle tissue which causes changes to the tissue, and these tissue changes allow extra fluid to drain out of the eye. IOP will be lowered over a couple of months.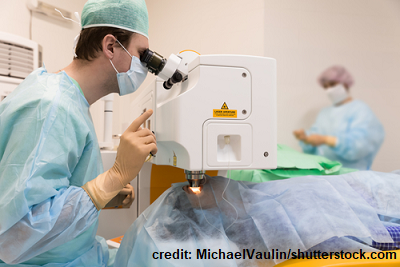
- Not permanent treatment…results last for several years.
Trabeculectomy (one common type): decreases IOP pressure in the eyes (used when eye drops or other procedures are not working)
- Some of the trabecular meshwork is removed and an opening is created to allow aqueous humour to collect in an area of the conjunctiva and this fluid will be reabsorbed and decrease eye pressure. The patient will have what’s called a bleb (pictured below) usually under the upper eyelid where the fluid has collected.
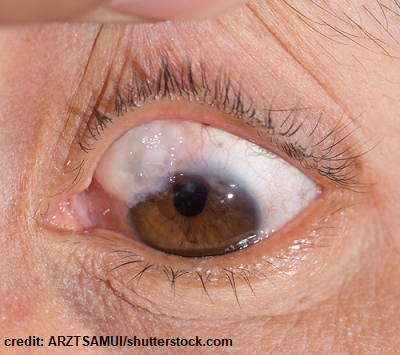
- Vision lost already will not come back…helps control pressure for several years not permanent.
General post-op education points after glaucoma surgery (patient education):
- Keep post-op appts. (very important because eye pressure is monitored along with other important post-op assessments)
- No driving until cleared by doctor.
- Protective sunglasses when in the direct sunlight.
- Instill eye drops exactly as prescribed (antibiotics/anti-inflammatory) and use clean hands.
- Don’t rub eyes, use contact lenses, and avoid activities that increase eye pressure: bending, straining activities like reading or straining during bowel movement (may need stool softeners), or lifting heavy objects
- Wear eye shield as prescribed.
- Blurred vision, eyes tear up more frequently, and eyes feeling itchy (stitches) are normal after procedure but will decrease overtime….report any sudden vision loss or severe pain….some pain is common.
- Monitor for signs of infection: discharge, fever, extreme eye redness and vision changes
Helpful to remember the 3 S’s of open-angle glaucoma (know the different signs and symptoms between open and closed-angle glaucoma):
- Silent Sight Stopper
- Silent (open-angle): asymptomatic until it’s too late because the irreversible damage has been done to the optic nerve when the patient notices loss of peripheral vision or tunnel vision.
- Sight: vision lost can’t be brought back and once blindness occurs it’s permanent…why it occurs? Increase intraocular pressure damages the optic nerve.
- Stopper: the development of permanent vision loss/blindness is stoppable (hence avoidable) if glaucoma is identified early through an exam eye that checks for eye pressure (help prevent the loss of vision through medications or procedures to keep IOP low)…know the risk factors for glaucoma…discussed below.
Immediate treatment for angle-closure glaucoma (emergency): remember this type is NOT silent with its symptoms (patient will report symptoms as noted above)
- Mediations: eye drops and oral medication to drop eye pressure along with
- Surgical procedure:
- laser iridotomy: small hole created in the iris with a laser to drain the increased aqueous humour
- Iridectomy: removes part of the iris)
- may be performed in both eyes because of the risk of the other eye developing angle-closure as well.
Eye gtts (drops)
General guidelines for administering eye drops (we have a video that gives step-by-step demonstration):
- Stress to the patient the importance of using eye drops exactly as ordered (don’t skip days or abruptly stop)….these medications can help stop the progression of blindness associated with glaucoma
- Use clean hands
- Administering more than 1 type of eye drop medication?
- Space out giving the medications: administer about 3-5 minutes apart so that the first medication can be used by the eye and not washed out by the second medication (very important)
- Eye ointment or eye drops first? Drops then ointment
- Drops are placed into the lower sac of the eye (conjunctival sac)….NOT directly on the eye via the cornea (observe the patient using the drops and re-educate if using incorrectly)
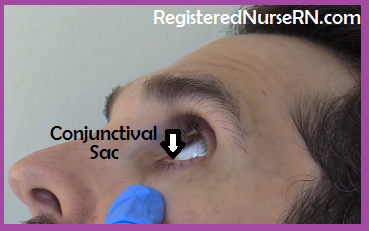
- After instilling each eye drop medication have the patient refrain from blinking but keep the eye closed and perform “punctal occlusion”.

- Use the index finger and gently place pressure at the side of the bridge of the nose (over the tear duct) for about 2-3 minutes.
- WHY? Prevents the medication from draining down into the nasolacrimal duct and being absorbed by the bloodstream, and it allows more medication to stay in the eye to work. This can happen with beta blockers, cholinergics, and other eye drop medications.
Eye medications: help lower intraocular pressure (decrease production of aqueous humour and/or increase drainage of aqueous humour from the eye)
To help us remember 4 groups of glaucoma meds, let’s remember the ABCC’s:
Alpha agonists “idine”: Brimonidine: works with alpha receptors by activating them….decreases aqueous humour production (constriction to the ciliary body) and helps increase the drainage of aqueous out of the eye and this lowers IOP.
- Systemic effects: punctal occlusion very important
- Risk of feeling very drowsy
Beta blockers “olol”: Timolol: decrease aqueous humour production
- Systemic effects, cardioselective & noncardioselective types
- not for patients with bradycardia, asthma, or COPD
- assess breathing and heart rate before administration
Carbonic anhydrase Inhibitors (CAIs): “zolamide” (oral or drops): “Acetazolamide”
- Decrease aqueous humour production…diuretic that inhibits carbonic acid production
- Assess for a sulfonamide allergy
Cholinergic (miotics): “Pilocarpine” eye drops: helps lower intraocular pressure especially in angle-closure glaucoma
- How? They constrict the pupil which will help increase drainage of aqueous humour out through the trabecular meshwork.
- Antidote is atropine.
- Cholinergic effects: sweating, increase salivation, bronchospams, decreased heart rate etc. increase eye sensitivity to light (problems with vision in dim light especially)
- Punctal occlusion during administration
Prostaglandin analogs: “prost”: Bimatoprost
- increase the drainage of aqueous humour out of the eye…doesn’t cause as many systemic effects as the other medications but can lead to longer and thicker eyelashes and change color of iris to brown.
Rho kinase inhibitors (newer type of medications for glaucoma): Netarsudil:
- increase drainage of aqueous humour by inhibiting the ROCK pathway which is found in the trabecular meshwork so it will drain better and help decrease IOP .
- causes dilation: common side effect is conjunctival hyperemia (extremely red eyes)
*these drugs can be combined…example: beta blocker w/ alpha agonist etc.
Factors that increase the development of glaucoma: SAVE your eyesight!
- Sixty or older (especially w/ family history)
- African American, Hispanic, and Asian Community
- Vascular Problems (diabetes, hypertension etc.)
- Elevated intraocular pressure (generally normal IOP 10-21 mmHg)
References:
Glaucoma | National Eye Institute. (2020). Retrieved 19 November 2020, from https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/glaucoma
Glaucoma Awareness Month. (2020). Retrieved 19 November 2020, from https://www.cdc.gov/features/glaucoma-awareness/index.html