This NCLEX review will discuss cystic fibrosis.
As a nursing student, you must be familiar with cystic fibrosis and how it affects the pediatric and adult population. In addition to the signs and symptoms, nursing interventions, and treatments for this condition.
Don’t forget to take the free quiz that contains cystic fibrosis nclex questions after reviewing this material.
Cystic Fibrosis Lecture
Cystic Fibrosis NCLEX Review
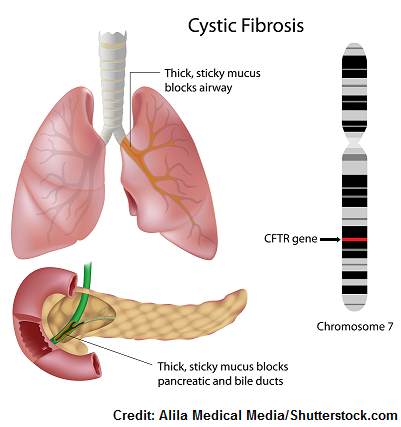 What is cystic fibrosis? It’s a genetic disorder that causes the EXOCRINE glands to work incorrectly. This leads to some major complications that can affect the respiratory (both upper/lower), digestive (pancreas, liver, intestines), integumentary, and reproductive systems.
What is cystic fibrosis? It’s a genetic disorder that causes the EXOCRINE glands to work incorrectly. This leads to some major complications that can affect the respiratory (both upper/lower), digestive (pancreas, liver, intestines), integumentary, and reproductive systems.
What are exocrine glands? These are glands that produce and transfer it’s secretions (ex: mucous, tears, sweat, digestive enzymes) via DUCTS to its intended area of the body rather than directly into the bloodstream like endocrine glands.
In cystic fibrosis, a gene that makes up the exocrine glands is mutated and this prevents the exocrine glands from working properly. The gene that is mutated is called the CFTR gene!
The CFTR gene, which stands for cystic fibrosis transmembrane regulator, is a protein that controls the channels of sodium and chloride. In other words, it controls the sodium and water transport in and out of the cell.
Therefore, these channels that are within the membrane of exocrine cells that makes our sweat, mucous, tears, and digestive enzymes don’t work properly. So, the substances produced by the exocrine glands don’t look and work like they are supposed to.
For example: How is mucous supposed to be? Thin and slippery which helps lubricate the structures. However, this is the problem in patients with cystic fibrosis.
- In patients with CF the mucous is THICK and STICKY (rather than thin and slippery) and this affects the following structures:
- Lungs (upper and lower):
- upper sinuses and formation of polyps (leading to snoring, nasal stuffiness)
- blockage of the airways: overtime leads to obstructive pulmonary diseases like emphysema …..air trapping can occur which causes hyperinflation
- Or bleds can develop and rupture leading to a pneumothorax
- Pulmonary hypertension which can lead to heart failure in the long term
- Clubbing of the nails due to the lack of oxygen in the blood
- Hemoptysis: coughing up blood either due to infection or severe damage to lung tissue (mainly in older patients rather than children)
- Very susceptible to lung infections that can create permanent damage to the lungs
- Thick, sticky mucous creates perfect conditions for bacteria to thrive and survive! These patients are at risk for pseudomonas aeruginosa, staphylococcus aureus etc.
- There is a risk of the development of antibiotic resistance or allergies to antibiotics, which can make treating the infection very hard.
- Gastrointestinal (blockage of passage ways within the body)
- Pancreas (this structure makes pancreatic enzymes):
- PAL: protease, amylase, lipase: These substances are secreted via the pancreatic duct into the duodenum and this helps digest proteins, fats, and vitamins.
- However, these enzymes are not accessible for proper usage because of the mucous blocking the pancreatic duct. Hence, they will stay in the pancreas and this inflames the structure and can cause fibrosis of the pancreas. In addition, the patient can develop cystic fibrosis related diabetes. Therefore, when a patient is not receiving pancreatic enzymes they will experience:
- weight loss, malabsorption, nutrition major issue, delayed puberty, GREASY, ODOROUS STOOL, BLOATNG, ABODOMINAL PAIN
- Many patients will need a feeding tube to help with nutrition, PANCREATIC ENZYMES SUPPLEMENTS, fat-soluble vitamins like D E A K
- Liver: mucous blocks biliary ducts which causes the bile to become thick and gallstones can develop along with gallbladder inflammation.
- Distal Intestinal Obstruction Syndrome (DIOS): blockage in the intestine….intestines can also make thick mucus like the lungs and pancreas and when thick mucus and stool get together it can lead to a blockage in the gut.
- Meconium ileus (infants): sticky meconium becomes stuck in the ileum of the intestine
- Infertility in males and females: most people who have cystic fibrosis are unable to have children because of the thickness of mucous. For example, women have troubling conceiving because the cervical mucous is not friendly towards sperm, and males tend to be sterile because there are issues with the vas deferens duct that helps sperm go for the testicle to the urethra (thick mucus blocking it or the duct is not formed correctly).
- Integumentary: sweat glands produce too much salt. Therefore, the sweat/tears are very salty. The patient is at risk for electrolyte complications and dehydration. However, the salty sweat is helpful with diagnosing CF (sweat chloride test).
- Distal Intestinal Obstruction Syndrome (DIOS): blockage in the intestine….intestines can also make thick mucus like the lungs and pancreas and when thick mucus and stool get together it can lead to a blockage in the gut.
- Pancreas (this structure makes pancreatic enzymes):
- Thick, sticky mucous creates perfect conditions for bacteria to thrive and survive! These patients are at risk for pseudomonas aeruginosa, staphylococcus aureus etc.
- Lungs (upper and lower):
Quick Facts about Cystic Fibrosis:
- Most common is Caucasians and males, but can affect any race or gender.
- NIH (National Institute of Health) statistics: life expectancy in 1960 was age 10. Today the median life expectancy is age 37 (“NIH Fact Sheets – Cystic Fibrosis”, n.d.).
- This is most commonly detected during the 1st year of life…child will have GI and respiratory issues (ex: infant may have a meconium ileus).
- Severity depends (not all patients are 100% alike in their severity)
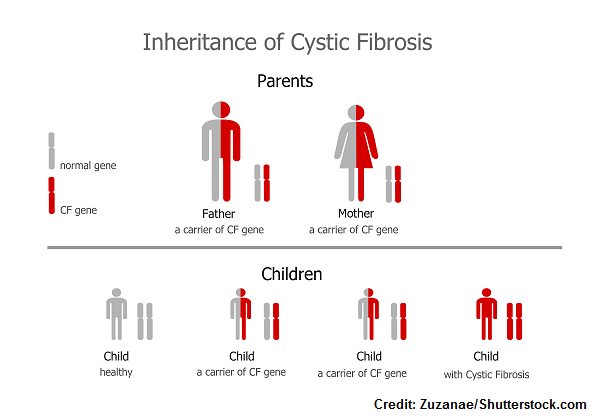
- It’s an autosomal recessive disorder….which means the child had to receive one mutated gene from both parents. In most cases, the parents are carriers of the disease but don’t have symptoms of CF.
- Diagnosed: Sweat Test: painless test that measures the amount of salt in the sweat
- Pilocarpine and electric current is applied to the skin to help it sweat (usually on the arm). A gauze is used to collect the sweat which is sent to a lab to measure the salt in the sweat
- Results:
- 39 mmol/L or less negative for cystic fibrosis
- 40 to 59 mmol/L needs further testing, not conclusive
- 60 mmol/L or more POSITIVE for cystic fibrosis
- Results:
- Pilocarpine and electric current is applied to the skin to help it sweat (usually on the arm). A gauze is used to collect the sweat which is sent to a lab to measure the salt in the sweat
Nursing Interventions and Treatments for Cystic Fibrosis
Nursing Focus: Mucous, Nutrition, Treatment for infection (most patients will die due to a lung infection or issue of some type), preventing blockages in GI system
Patients who have CF are on a wide variety of medications like the following:
- stool softeners
- pancreatic enzymes
- nasal sprays
- vitamins
- antibiotics
- anti-inflammatories (inhaled or oral)
- mucolytics (oral or nebulizer)
- bronchodilators (oral or inhaled)
Mucous: Huge part of the everyday routine treatment and this includes: Chest PT, postural drainage, using PEP devices and nebulizers along with huff coughing
- Chest physiotherapy (Chest PT): helps drain the airways of that thick sticky mucous
- It is done with postural drainage along with percussion and vibration to facilitate the draining of mucous from the lung lobes followed by huff coughing (THIS IS A HUGE PART OF treatment for CF patients!!!!)
Chest PT: percussion (cupping hands and percussing of the over the lung fields and take special care when percussing over spine, stomach, breast bone, organs to avoid injury), some patients use vibration with a special vest and then huff coughing is performed
**Patient usually performs this 2-4 times per day or more depending on if they are fighting a lung infection. Sessions vary: 20 minutes to an hour.
TEST!!! When should you perform chest PT on a patient? Perform when the stomach is empty to prevent reflux of food and vomiting……1-2 hours after meals (hence in between meals). NOT after (reason: regurgitation) or before (reason: risk of decreasing the appetite because coughing up thick sticky mucous can taste bad which can decrease a person’s appetite).
Airway Clearance devices: PEP (positive expiratory pressure): Helps with clearing the airway
- PEP devices: assists with moving mucous from the lungs…..person breathes in and out of device (resistance when breathing out and this helps even more to move mucous)….creates a vibration (performs several times) and then huff cough to expel mucous. Device names: Flutter valve or Acapella
Prevent infection: wearing a mask due flu times or when sick, hand hygiene, avoid sick people, and stay up-to-date with vaccinations, lung transplant possible if lung problems severe
Exercise: regular aerobic exercise to help keep lungs healthy and clear secretions. Educate to monitor sweating because of the risk of losing too much salt (may need salt supplements and increase caloric needs when exercising)
GI: pancreatic enzymes, fat-soluble vitamins, high calories, high protein and high fat diet
Pancreatic enzymes:
TEST!!! Swallow them! Don’t chew or crush them! If person can’t swallow the capsule, you can open it and put it in an ACIDIC FOOD like apple sauce. Do not mix in an alkaline-based food like yogurt, pudding or ice cream because this will inactive the enzyme.
How do you know the patient is receiving an adequate amount of enzymes? The patient’s stool is NOT greasy or odorous and they are free from abdominal bloating or pain.
TEST!!! When would you administer these enzymes? Administer before all meals and snacks. Example of these enzymes are: Pancrelipase, Pancreatin
Some patients have feeding tubes because their caloric intake is very high, especially during illness or during the late stages of the disease. High protein and high calorie and fat diet with vitamin supplements like the fat-soluble: DEKA
Obstruction and Constipation Prevention
- Drink a lot of water to keep mucous in gut thin, use Miralax Polyethylene Glycol (common) daily as prescribed by MD to prevent constipation
- Monitor for bowel obstruction: signs: no bowel movement, pain, can’t pass gas etc.
Cystic Fibrosis Diabetes Mellitus: pancreas is damaged….monitor blood sugar (can drop or be high)…may need insulin
Nurse Sarah’s Notes and Merch
Just released is “ABG Interpretation Notes, Mnemonics, and Workbook by Nurse Sarah“. These notes contain 64 pages of Nurse Sarah’s illustrated, fun notes with mnemonics, and worksheets that include over 90 ABG practice problems and 60 test review questions covering ABG concepts.
You can get an eBook version here or a physical copy of the book here.

References:
Cystic Fibrosis | National Heart, Lung, and Blood Institute (NHLBI). Retrieved from https://www.nhlbi.nih.gov/health-topics/cystic-fibrosis
NIH Fact Sheets – Cystic Fibrosis. Retrieved from https://report.nih.gov/NIHfactsheets/ViewFactSheet.aspx?csid=36
U.S. Department of Health and Human Services. Facts about Cystic Fibrosis[Ebook] (pp. 3-5). Retrieved from https://www.cdc.gov/scienceambassador/documents/cystic-fibrosis-fact-sheet.pdf